Last updated on April 25th, 2026 at 05:35 am
Medically responsible content note:
This article is for education only and does not diagnose or treat medical, dental, or sleep conditions. Bruxism, jaw pain, headaches, snoring, breathing pauses, and respiratory symptoms can have multiple causes. Seek care from a qualified medical, dental, sleep, or orofacial pain professional when symptoms are persistent, worsening, severe, or disruptive.
Asthma and allergies often overlap. You may notice coughing, wheezing, chest tightness, sneezing, nasal congestion, itchy eyes, or trouble breathing after exposure to pollen, dust, pets, mold, smoke, exercise, strong odors, or weather changes. For some people, these symptoms are mild and seasonal. For others, they affect sleep, energy, exercise, work, school, and daily life.
Asthma affects the airways in your lungs. Allergies involve your immune system reacting to substances that are usually harmless to most people. When these two conditions happen together, allergens may irritate the nose, throat, and lungs. This can make breathing symptoms worse, especially at night.
You will learn how asthma and allergies are connected, which symptoms and triggers matter, how these conditions can affect sleep, and when to ask a healthcare provider for help.
Editor’s note: This article is for patient education only. It does not diagnose asthma, allergies, or sleep-related breathing disorders. If breathing symptoms are severe, worsening, or disrupting sleep, speak with a qualified healthcare provider.
Quick Answer: How Are Asthma and Allergies Connected?
Asthma and allergies are connected because allergens can irritate the airways and trigger asthma symptoms in some people. Pollen, dust mites, mold, pet dander, and cockroach particles may cause sneezing, congestion, itchy eyes, coughing, wheezing, chest tightness, or shortness of breath. If asthma and allergy symptoms happen together, both conditions should be discussed with a healthcare provider.
What Is Asthma?
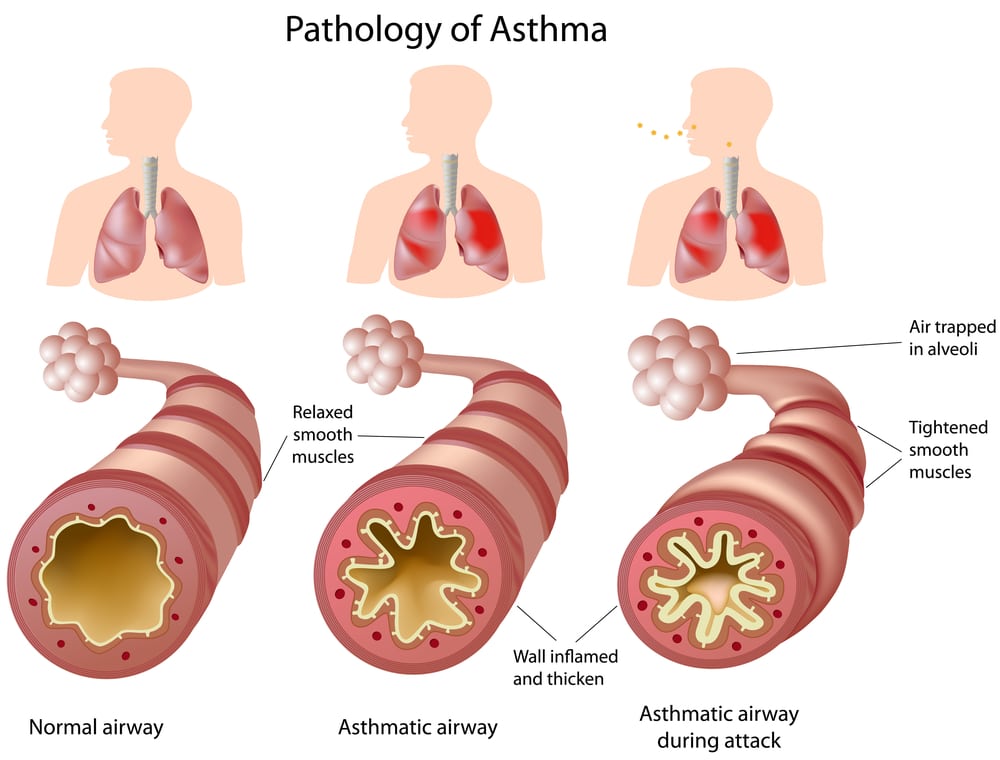
Asthma is a chronic respiratory condition that affects the airways in your lungs. When you have asthma, your airways may become inflamed, swollen, narrow, and more sensitive to triggers. This can make it harder for air to move in and out of your lungs.
Asthma symptoms can come and go. Some people only notice symptoms during exercise, allergy season, respiratory infections, or exposure to smoke or cold air. Others have more persistent symptoms that require daily management.
Asthma can affect people of all ages. It may begin in childhood, but adults can develop asthma too. Because symptoms can overlap with other breathing problems, asthma should be evaluated by a healthcare provider.
Common Asthma Symptoms
Asthma symptoms can look different from person to person. Some people wheeze. Some mainly cough. Others feel tightness in the chest or become short of breath during activity.
Common asthma symptoms include:
- Wheezing, or a whistling sound when breathing
- Shortness of breath
- Chest tightness or chest pressure
- Coughing, especially at night or early in the morning
- Trouble exercising because of breathing symptoms
- Waking up because of coughing, wheezing, or breathlessness
- Symptoms that worsen around smoke, pollen, pets, cold air, or strong odors
Nighttime coughing or wheezing is especially important. If asthma symptoms wake you up, your asthma may not be well controlled.
Common Types of Asthma
Asthma can be grouped in different ways based on triggers and symptom patterns.
Allergic Asthma
Allergic asthma is triggered by allergens such as pollen, dust mites, mold, pet dander, or cockroach particles. This is one of the clearest links between allergies and asthma. When your immune system reacts to an allergen, your airways may also become irritated.
Non-Allergic Asthma
Non-allergic asthma is triggered by irritants or conditions that are not classic allergens. These may include smoke, air pollution, cold air, respiratory infections, exercise, stress, or strong odors.
Exercise-Induced Asthma
Exercise-induced asthma causes symptoms during or after physical activity. You may notice coughing, wheezing, chest tightness, or shortness of breath. Exercise is important for health, so symptoms should be discussed with a healthcare provider rather than ignored.
Occupational Asthma
Occupational asthma is triggered by exposures at work. Possible triggers include chemicals, dust, fumes, cleaning products, animal proteins, wood dust, or industrial materials. If symptoms improve away from work and worsen during workdays, tell your healthcare provider.
What Are Allergies?
Allergies happen when your immune system reacts to a substance that is usually harmless to most people. These substances are called allergens.
Common allergens include:
- Pollen
- Dust mites
- Mold
- Animal dander
- Certain foods
- Insect stings
- Some medications
When your body reacts to an allergen, it releases chemicals such as histamine. This can cause symptoms in the nose, eyes, skin, throat, lungs, or digestive system.
Common Allergy Symptoms
Allergy symptoms depend on the allergen and how your body reacts. Some allergies are mild and annoying. Others can be serious.
Common allergy symptoms include:
- Sneezing
- Runny nose
- Stuffy nose
- Itchy, watery eyes
- Postnasal drip
- Coughing
- Skin rash or hives
- Itching
- Swelling of the lips, face, tongue, or throat
- Trouble breathing in more serious reactions
Allergy symptoms can also affect sleep. Nasal congestion, postnasal drip, coughing, and mouth breathing may make it harder to sleep comfortably.
Common Types of Allergies
Allergies can affect different parts of the body and may be triggered by different exposures.
Seasonal Allergies
Seasonal allergies, often called hay fever or allergic rhinitis, are commonly triggered by pollen from trees, grasses, or weeds. Symptoms may worsen during certain seasons.
Indoor Allergies
Indoor allergies may be triggered by dust mites, mold, pet dander, or cockroach particles. These triggers can be especially important because people spend many hours indoors, including while sleeping.
Food Allergies
Food allergies happen when the immune system reacts to a specific food. Common food allergens include peanuts, tree nuts, shellfish, milk, eggs, soy, wheat, and fish. Food allergies can sometimes cause severe reactions and should be diagnosed and managed with medical guidance.
Insect Sting Allergies
Some people react strongly to stings from bees, wasps, hornets, or yellow jackets. These reactions can range from local swelling to a severe whole-body allergic reaction.
Drug Allergies
Drug allergies are reactions to certain medications. If you suspect a medication allergy, talk with a healthcare provider before taking that medication again.
How Are Asthma and Allergies Connected?
Asthma and allergies are closely related. Many people with asthma also have allergies. Allergies can trigger asthma symptoms, and asthma can make breathing symptoms more serious when allergic reactions affect the airways.
For example, dust mites may cause sneezing, congestion, and itchy eyes. In someone with allergic asthma, that same exposure may also trigger coughing, wheezing, chest tightness, or shortness of breath.
Common allergens that may trigger asthma symptoms include:
- Pollen
- Dust mites
- Mold
- Pet dander
- Cockroach particles
If you have both asthma and allergies, managing only one condition may not be enough. Better allergy control may help reduce asthma flare-ups. Better asthma control may make breathing safer when allergies worsen.
Common Asthma and Allergy Triggers
Triggers are not the same for everyone. One person may react strongly to pollen, while another reacts to cold air, exercise, smoke, or cleaning products. Learning your own triggers is one of the most useful steps in managing asthma and allergies.
Outdoor Triggers
Outdoor triggers may include:
- Pollen
- Mold spores
- Air pollution
- Wildfire smoke
- Cold air
- Weather changes
Indoor Triggers
Indoor triggers may include:
- Dust mites
- Pet dander
- Mold
- Cockroach particles
- Tobacco smoke
- Strong fragrances
- Cleaning chemicals
- Poor ventilation
Lifestyle and Activity Triggers
Some symptoms may be triggered by:
- Exercise
- Respiratory infections
- Stress
- Laughing or crying hard
- Cold drinks or cold air exposure
- Poor sleep
- Skipping prescribed medication
Workplace Triggers
Workplace triggers may include:
- Dust
- Fumes
- Chemicals
- Cleaning products
- Smoke
- Animal exposure
- Industrial materials
If symptoms follow a pattern, write it down. Patterns can help your healthcare provider adjust your treatment plan.
How Asthma and Allergies Can Affect Sleep
Asthma and allergies can make sleep harder. This is one reason these conditions matter in respiratory health. Breathing problems do not only affect daytime comfort. They can also affect how well you sleep and how rested you feel the next day.
Allergies can cause nasal congestion, postnasal drip, mouth breathing, dry mouth, coughing, and snoring. Asthma can cause nighttime coughing, wheezing, chest tightness, or shortness of breath. Some people wake up during the night because they cannot breathe comfortably.
Nighttime symptoms are important because they may suggest that asthma, allergies, nasal obstruction, or another breathing problem is not well controlled.
Talk with a healthcare provider if you regularly experience:
- Waking up coughing
- Wheezing at night
- Shortness of breath during sleep
- Chest tightness in bed
- Heavy nasal congestion at night
- Mouth breathing or dry mouth in the morning
- Loud or frequent snoring
- Daytime fatigue after a full night in bed
Better control of asthma and allergies may improve sleep quality.
If you also wake up with dry mouth, mouth breathing, or snoring, you may want to read our guide to mouth breathing at night.
If snoring, choking, gasping, or severe daytime sleepiness is present, read our guide to Understanding Sleep Disorders; Beyond Just Fatigue
How Doctors Diagnose Asthma and Allergies
Asthma and allergies can share symptoms with other conditions. Coughing, congestion, shortness of breath, and chest tightness can have several causes. That is why diagnosis matters.
A healthcare provider may use:
- A detailed symptom history
- A physical exam
- Lung function testing
- Peak flow measurements
- Allergy skin testing
- Blood tests for allergy markers
- Review of medication use
- Review of home, work, and environmental exposures
Asthma diagnosis often involves testing how well your lungs move air. Allergy diagnosis may involve identifying specific substances that trigger immune reactions. In some cases, your provider may refer you to an allergist, pulmonologist, or another specialist.
The goal is not just to name the condition. The goal is to understand what is driving your symptoms so your treatment plan matches your triggers and risks.
For a deeper look at sleep-related breathing problems, read our guide to shallow breathing during sleep and hypopnea.
Asthma and Allergy Treatment Options
Managing asthma and allergies usually involves a combination of trigger control, medication, monitoring, and follow-up care. Your plan should be based on your diagnosis, symptom severity, health history, and daily exposures.
Avoid Known Triggers When Possible
Avoiding triggers can reduce symptoms and lower the risk of flare-ups. This does not mean you can avoid every trigger all the time. The goal is to reduce exposure where it is realistic.
Helpful steps may include:
- Keeping windows closed during high-pollen days
- Using air conditioning when pollen or pollution is high
- Washing bedding regularly
- Reducing dust in the bedroom
- Using allergen-resistant pillow and mattress covers
- Controlling indoor humidity if mold is a problem
- Avoiding tobacco smoke
- Limiting strong fragrances and harsh cleaning products
- Keeping pets out of the bedroom if pet dander is a trigger
- Using protective equipment at work when advised
Small environmental changes can make a meaningful difference, especially when symptoms are frequent.
Medications for Asthma and Allergies
Several types of medications may be used to manage asthma and allergies. Your provider will decide what is appropriate for you.
Asthma medications may include:
- Inhaled corticosteroids to reduce airway inflammation
- Bronchodilators to relax airway muscles
- Rescue inhalers for quick symptom relief
- Controller medications for long-term management
- Combination inhalers for some patients
Allergy medications may include:
- Antihistamines
- Nasal corticosteroid sprays
- Decongestants when appropriate
- Eye drops
- Leukotriene modifiers
- Other prescription allergy treatments
Take medications exactly as prescribed. If a medication is not helping, causes side effects, or is difficult to use, do not simply stop without guidance. Talk with your healthcare provider so your plan can be adjusted safely.
Allergy Shots and Immunotherapy
Allergy shots, also called immunotherapy, may be an option for some people with allergies. Immunotherapy works by exposing the body to small, controlled amounts of an allergen over time. The goal is to help the immune system become less reactive.
This treatment is not right for everyone, and it takes time. However, for selected patients, it may help reduce allergy symptoms and may also help some people whose asthma is triggered by allergies.
Ask your healthcare provider or allergist whether immunotherapy is appropriate for your situation.
How to Create an Asthma and Allergy Action Plan
An asthma and allergy action plan is a written plan that tells you what to do when symptoms are controlled, when they are getting worse, and when you need urgent help. This is especially important if you have asthma attacks, severe allergies, or symptoms that change quickly.
A useful action plan may include:
- Your daily medications
- How and when to use a rescue inhaler
- What symptoms mean your condition is worsening
- Peak flow instructions, if your provider recommends them
- What to do during an asthma flare-up
- What to do during an allergic reaction
- When to call your healthcare provider
- When to go to urgent care or the emergency room
- Emergency contact information
Keep your plan where you can find it. Share it with family members, caregivers, school staff, coaches, or coworkers if appropriate.
How to Track Symptoms and Triggers
A simple symptom diary can help you and your provider identify patterns. You do not need a complicated system. A notebook, phone note, or printed tracker can work.
Consider tracking:
- Coughing
- Wheezing
- Shortness of breath
- Chest tightness
- Sneezing or congestion
- Itchy or watery eyes
- Nighttime waking
- Snoring or mouth breathing
- Medication use
- Exercise
- Weather changes
- Pollen levels
- Pet exposure
- Smoke or fragrance exposure
- Cleaning product exposure
- Food reactions
- Workplace exposures
Also write down when symptoms improve. This can help show which treatments or avoidance strategies are working.
Bring your notes to medical appointments. Real-world symptom patterns can help your provider make better decisions.
If you are tracking oxygen levels or sleep breathing data, this article explains why SpO2 is useful but not diagnostic on its own.
When Asthma or Allergies Need Medical Attention
Some asthma and allergy symptoms require prompt medical care. Do not ignore breathing symptoms that are severe, worsening, or not responding to your usual treatment plan.
Seek urgent medical help if you have:
- Severe shortness of breath
- Trouble speaking in full sentences
- Blue or gray lips or fingernails
- Chest tightness that does not improve
- Wheezing or breathing trouble that worsens quickly
- Confusion, faintness, or extreme weakness
- Swelling of the tongue, lips, throat, or face
- Trouble swallowing or breathing after exposure to a food, medication, or insect sting
- Symptoms of anaphylaxis
- Rescue medication that is not helping as expected
If you already have an asthma or allergy action plan, follow it. If symptoms feel severe or life-threatening, seek emergency care immediately. If you are unsure whether breathing symptoms are serious, it is safer to seek medical advice promptly rather than wait.
Living Well with Asthma and Allergies
Living with asthma and allergies can be frustrating. Symptoms may interrupt sleep, exercise, work, travel, social plans, and family routines. The goal is not just to push through. The goal is to understand your condition and create a plan that helps you live more comfortably and safely.
Build Support Around Your Plan
Let the people close to you know what triggers your symptoms and what to do if you have a flare-up. This may include family members, friends, teachers, coaches, coworkers, or travel companions.
Protect Your Sleep
If congestion, coughing, wheezing, or mouth breathing disrupts your sleep, tell your healthcare provider. Sleep disruption can affect mood, concentration, energy, and quality of life. Nighttime symptoms are also important clues about how well your asthma and allergies are controlled.
Plan Ahead for Travel
If you are traveling, pack your medications, action plan, and any emergency supplies your provider recommends. Check pollen, weather, air quality, and possible exposures at your destination. If you have severe allergies, ask your healthcare provider what precautions you should take before traveling.
Take Care of Your General Health
Healthy routines can support your respiratory health. Try to get enough sleep, stay physically active within your medical limits, eat a balanced diet, and manage stress. If exercise triggers symptoms, ask your provider how to exercise more safely rather than avoiding activity altogether.
Frequently Asked Questions About Asthma and Allergies
Can allergies make asthma worse?
Yes. Allergies can trigger asthma symptoms in some people. When your immune system reacts to an allergen such as pollen, dust mites, mold, or pet dander, that reaction may also irritate your airways. This can lead to coughing, wheezing, chest tightness, or shortness of breath. If your asthma gets worse during allergy season or around certain indoor triggers, talk with your healthcare provider about managing both conditions together.
How do I know if my cough is from asthma or allergies?
A cough from allergies may come with sneezing, congestion, itchy eyes, or postnasal drip. A cough from asthma may come with wheezing, chest tightness, shortness of breath, or nighttime waking. However, the two can overlap. A healthcare provider can help determine whether your cough is related to allergies, asthma, reflux, infection, sinus problems, or another condition.
Can asthma symptoms get worse at night?
Yes. Some people with asthma notice more coughing, wheezing, chest tightness, or shortness of breath at night. Nighttime symptoms may mean asthma is not well controlled. Allergies can also worsen sleep by causing congestion, mouth breathing, coughing, or postnasal drip. If breathing symptoms regularly wake you up, discuss this with your healthcare provider.
Can allergies cause shortness of breath?
Yes. Allergies can contribute to shortness of breath in some people, especially if they trigger asthma symptoms or cause significant airway irritation. Nasal congestion can also make breathing feel more difficult. Sudden, severe, or worsening shortness of breath should be evaluated urgently.
Can asthma and allergies make you tired?
Yes. Asthma and allergies can make you tired when they disrupt sleep, increase nighttime coughing, cause congestion, or make breathing more difficult. Fatigue can also occur when symptoms are poorly controlled or when breathing problems wake you during the night.
Are allergy shots helpful for asthma?
Allergy shots may help some people whose asthma symptoms are triggered by allergies. They are not appropriate for everyone, and they require medical supervision. If allergy testing shows clear triggers and your symptoms are difficult to manage, your provider may refer you to an allergist to discuss immunotherapy.
What is an asthma action plan?
An asthma action plan is a written plan that explains how to manage your asthma day to day and what to do when symptoms get worse. It may include daily medications, rescue inhaler instructions, symptom zones, peak flow guidance, emergency steps, and when to seek medical care. Every person with asthma should ask their provider whether an action plan is appropriate.
Can indoor air quality affect asthma and allergies?
Yes. Indoor air can contain dust mites, mold, pet dander, smoke, fragrances, cleaning chemicals, and other irritants. These can worsen allergy and asthma symptoms in sensitive people. Improving bedroom air quality, reducing dust, controlling humidity, and avoiding indoor smoke may help reduce symptoms.
When should I see a doctor for asthma or allergy symptoms?
You should see a healthcare provider if symptoms are frequent, worsening, interfering with sleep, limiting exercise, requiring frequent rescue medication, or affecting daily life. You should seek urgent help for severe breathing trouble, swelling of the tongue or throat, symptoms of anaphylaxis, blue lips or fingernails, or symptoms that do not improve with your prescribed rescue treatment.
Conclusion
Asthma and allergies are common, but they should not be ignored when they affect breathing, sleep, energy, or quality of life. These conditions often overlap. Allergies may inflame the nose, throat, and airways. Asthma may make the lungs more sensitive to triggers. Together, they can lead to coughing, wheezing, congestion, chest tightness, nighttime waking, and difficulty staying active.
The most important step is understanding your personal pattern. What triggers your symptoms? Do they happen during pollen season? Around pets? At work? After exercise? In bed at night? During respiratory infections? When you track these details, you give your healthcare provider better information and help build a more effective plan.
Good asthma and allergy care usually includes diagnosis, trigger control, medication when needed, an action plan, and follow-up. It may also include allergy testing, lung function testing, immunotherapy, or specialist care.
If symptoms affect your sleep, that should be part of the conversation. Nighttime coughing, congestion, wheezing, mouth breathing, or shortness of breath can be signs that your respiratory health needs more attention.
With the right plan, many people with asthma and allergies can breathe better, sleep better, exercise more safely, and feel more confident in daily life. Start by paying attention to your symptoms, writing down your triggers, and working with a healthcare provider who can help you manage both conditions together.
References
American Academy of Allergy, Asthma & Immunology. Asthma.
American College of Allergy, Asthma & Immunology. Allergy Overview.
Centers for Disease Control and Prevention. Asthma.
Mayo Clinic. Allergies.
Randy Clare is a writer, educator, and health communicator focused on making complex clinical topics easier to understand. Through The Sleep and Respiratory Scholar, he creates clear, practical content on bruxism, headache, sleep, airway health, and respiratory symptoms. He is the author of The Brux Method, President of ClenchAlert.com and host of The Clenching Chronicle Podcast, where he explores jaw tension, clenching, headaches, and behavior-based approaches to relief. His work helps readers better understand symptoms, recognize patterns, and take more informed next steps.





