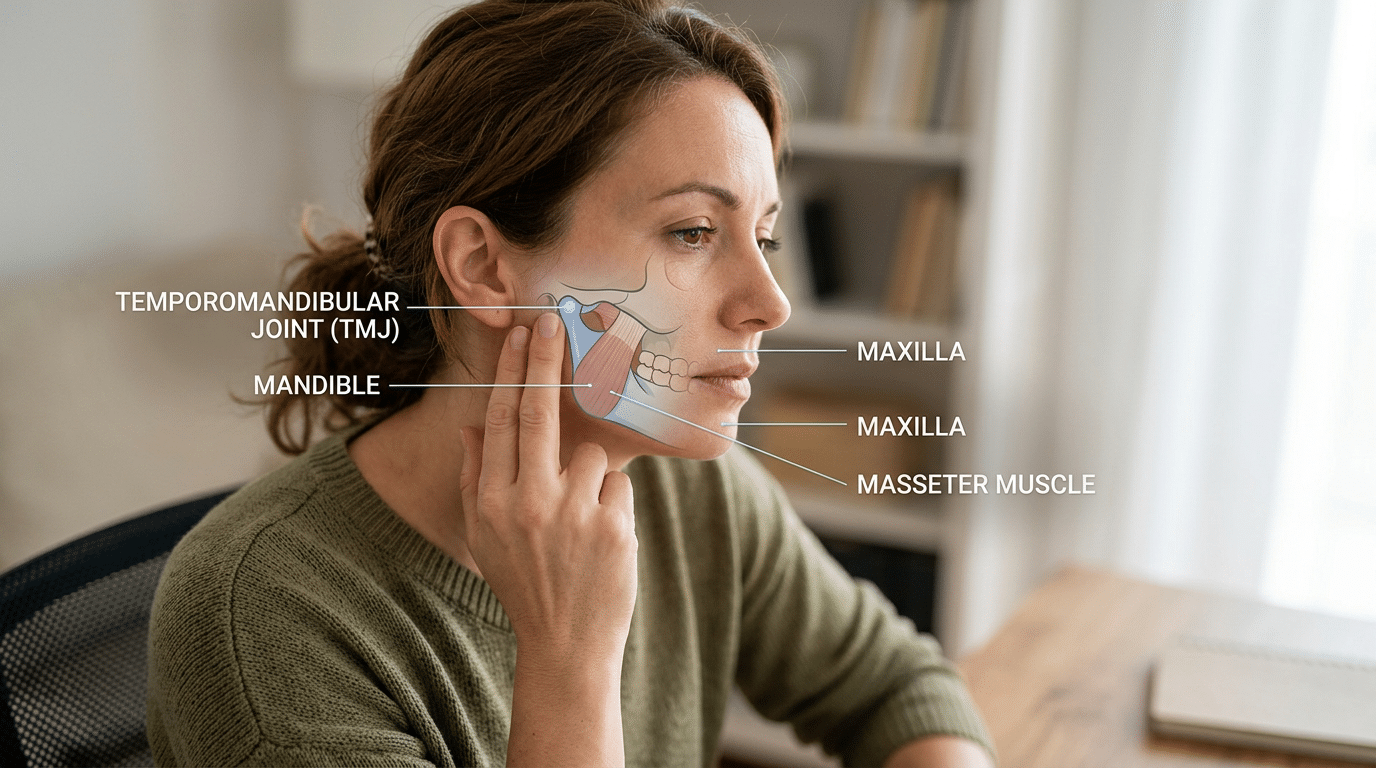
You may think you have a headache problem. But if your temples ache, your ears feel full, your teeth feel sore, or your jaw feels tired, your jaw joint may be part of the story.
Medically responsible content note:
This article is for education only and does not diagnose or treat medical, dental, or sleep conditions. Bruxism, jaw pain, headaches, snoring, breathing pauses, and respiratory symptoms can have multiple causes. Seek care from a qualified medical, dental, sleep, or orofacial pain professional when symptoms are persistent, worsening, severe, or disruptive.
A TMD headache can be confusing because the pain does not always stay in the jaw. It may show up in your temples, forehead, ears, cheeks, teeth, neck, or behind your eyes. That can make it feel like a sinus problem, earache, toothache, tension headache, or migraine. Many people describe this as a TMJ headache because the pain seems connected to the jaw joint.
This article will help you understand when the jaw may be part of a headache pattern, what symptoms to track, and when to ask for professional help.
Quick answer: What is a TMD headache?
A TMD headache is head, face, or neck pain linked to temporomandibular disorder. TMD can affect the jaw joints, chewing muscles, ligaments, nerves, and nearby structures. The National Institute of Dental and Craniofacial Research describes TMDs as more than 30 conditions that can cause pain and dysfunction in the jaw joint and chewing muscles.¹
A TMD headache can be felt in the temples, forehead, ears, cheeks, jaw, teeth, neck, or behind the eyes. It often gets worse with chewing, clenching, grinding, yawning, talking, stress, poor sleep, or prolonged jaw tension.
However, headaches can have many causes. A new, severe, changing, one-sided, or persistent headache should be evaluated by a qualified healthcare professional.
In one sentence:
A TMD headache happens when pain from the jaw joint, chewing muscles, or nearby nerves is felt as head, face, ear, tooth, or neck pain.
Featured snippet summary
TMD headache happens when pain from the jaw joint, chewing muscles, or nearby nerves is felt as head, face, ear, tooth, or neck pain. It can feel like temple pressure, ear pain, facial aching, or a tension-type headache. Pain that worsens with chewing, clenching, jaw movement, or morning jaw soreness may suggest the jaw is part of the pattern.
Key signs your headache may involve the jaw
A headache may involve TMD when it appears with:
- jaw soreness or fatigue
- temple tenderness
- pain that worsens with chewing
- clicking, popping, locking, or limited opening
- tooth soreness without a clear dental cause
- ear fullness without infection
- morning jaw pain or signs of clenching
For a broader guide to related symptoms, patterns, and next steps, visit the pillar article Headache and Facial Pain: How to Recognize Patterns and Know Who to Ask for Help.
What is TMD?
TMD stands for temporomandibular disorder. It describes problems involving the jaw joints, the chewing muscles, or both.
Your temporomandibular joints sit just in front of your ears. These joints help your jaw open, close, slide, and rotate. You use them when you chew, speak, yawn, swallow, laugh, and breathe through your mouth.
Here is the simplest way to remember the difference:
TMJ is the joint. TMD is the problem.
Many people search for “TMJ headache,” but the more accurate term is often “TMD headache” because the pain can come from the joint, the chewing muscles, or both. In everyday language, people often use both terms to describe headache pain linked to jaw problems.
TMD symptoms may include jaw pain, limited opening, clicking, popping, locking, chewing pain, earache, headache, and facial pain. A review in American Family Physician describes TMD as a group of musculoskeletal and neuromuscular conditions involving the TMJ complex and surrounding structures, with common symptoms that include jaw pain, earache, headache, and facial pain.²
How can jaw joint problems cause headache pain?
Pain does not always stay where it starts.
The jaw, face, head, ears, teeth, and neck share overlapping nerve pathways. When the jaw joint or chewing muscles are irritated, your brain can interpret the pain as coming from another nearby area.
That is called referred pain.
The jaw can act like a pain amplifier because it shares nerve pathways with the head, face, and neck.
Jaw-related headache pain can happen because:
- irritated jaw joints send pain signals into nearby facial pain pathways
- tight chewing muscles refer pain into the temples, forehead, cheeks, or teeth
- clenching and grinding overload the muscles, teeth, and joints
- neck tension and posture add strain to the jaw-head-neck system
- poor sleep and stress can make pain pathways more sensitive
The International Classification of Headache Disorders includes “headache attributed to temporomandibular disorder” as a recognized secondary headache category. Its criteria include clinical evidence of a painful process affecting the TMJ, chewing muscles, or related structures, along with evidence that the headache is linked to the TMD pattern.³
Where does TMD headache pain usually show up?
TMD-related pain can appear in several places. That is one reason it is often mistaken for something else.
Common locations include:
- temples
- forehead
- behind the eyes
- in front of or around the ears
- cheeks
- jaw angle
- teeth
- neck
- base of the skull
- one side of the head or both sides
The most important clue is not location alone. The pattern matters.
For example, temple pain that appears with jaw soreness, chewing pain, tooth sensitivity, jaw clicking, morning jaw fatigue, or daytime clenching can suggest that the jaw is part of the headache pattern. This is why a jaw joint headache may feel like temple pain, ear pain, tooth pain, or facial pressure.
If temple pain is your main symptom, the article on temple headaches explains other patterns to consider.
What does a TMD headache feel like?
Now that you know where TMD pain can show up, the next question is what it feels like.
A TMD headache may feel like:
- a dull ache in the temples
- pressure in the jaw, face, or head
- ear fullness or pain
- morning headache with jaw soreness
- tooth soreness without an obvious dental cause
- headache after a stressful workday
- pain that increases with chewing, talking, or yawning
- tenderness in the jaw muscles or temples
- facial fatigue
- neck stiffness with jaw tension
If pain changes when the jaw works harder, the jaw can be part of the pattern.
However, symptoms alone do not prove the cause. TMD headache can overlap with tension headache, migraine, sinus pain, dental pain, neck-related headache, and ear pain. In some people, more than one condition is present at the same time.
Why TMD pain can feel like ear pain, tooth pain, or sinus pressure
This is why TMD often sends people to the wrong first appointment. The symptoms can feel like they belong to the ear, teeth, sinuses, or neck.
TMD and ear pain
The TMJ sits just in front of the ear. When the joint or nearby muscles become irritated, pain can be felt around the ear, in front of the ear, or deep near the ear canal.
Some people also report ear fullness, pressure, or tenderness even when an ear exam does not show an infection. Still, ear symptoms should be checked by a medical professional when they are new, persistent, one-sided, or linked with hearing changes, drainage, dizziness, or fever.
If ear discomfort is part of your pattern, the guide to headache with ear pain explains why the jaw, ear, and head can overlap.
TMD and tooth pain
Clenching and grinding can make teeth feel sore, sensitive, or bruised. Sometimes the pain feels like it is coming from one specific tooth. Other times, several teeth feel tender.
Dental causes must be ruled out. Cavities, cracked teeth, gum disease, infections, and bite trauma can all create tooth pain. But when dental imaging and exams do not explain the pain, jaw muscle referral and clenching patterns may be part of the picture.
TMD and sinus-like pressure
Pain in the cheeks, upper teeth, under the eyes, or forehead can feel like sinus pressure. Sometimes it is. Sinus infection, allergies, nasal inflammation, and other medical issues can cause facial pressure.
However, jaw muscle referral can also create cheek, temple, and upper tooth discomfort. If the pain changes with chewing, clenching, jaw movement, stress, or jaw relaxation, the jaw may be involved.
TMD and neck pain
The jaw and neck do not work in isolation. Forward head posture, screen time, shoulder tension, mouth breathing, and stress bracing can all increase load on the jaw-neck system.
That is why some people feel jaw pain, temple pain, neck stiffness, and headache together.
What triggers a TMD headache?
For many people, the trigger is not one big event. It is repeated jaw loading throughout the day.
Common triggers include:
- jaw clenching
- teeth grinding
- stress
- long periods of concentration
- screen posture
- chewing gum
- hard or chewy foods
- wide yawning
- poor sleep
- sleep bruxism
- awake bruxism
- recent dental work
- bite changes
- neck tension
- trauma or injury
These triggers can stack. You may clench during work, chew gum in the afternoon, sleep poorly at night, and wake with sore jaw muscles the next morning. None of those triggers has to be extreme. Together, they can overload the jaw system.
NIDCR includes reducing habits such as jaw clenching, gum chewing, and nail biting among conservative strategies that may help some people with TMD symptoms.¹
TMD headache vs tension headache vs migraine
TMD headache can overlap with other headache types. Use this table as a pattern guide, not a diagnosis.
| Feature | TMD headache | Tension headache | Migraine |
|---|---|---|---|
| Common location | Temples, jaw, ears, face, neck | Both sides of head, forehead, neck | Often one-sided, eye, temple, or head |
| Pain quality | Aching, pressure, soreness | Tight, pressing, band-like | Throbbing, pulsing, intense |
| Jaw symptoms | Common | Sometimes | Sometimes |
| Worse with chewing | Often | Not usually | Possible, but less specific |
| Light sensitivity | Less typical | Usually absent or mild | Common |
| Sound sensitivity | Less typical | Usually absent or mild | Common |
| Nausea | Uncommon | Uncommon | Common |
| Morning symptoms | Common if bruxism or sleep issues are involved | Possible | Possible |
| Clicking or locking | May occur | Not typical | Not typical |
| Professional to consider | Dentist, orofacial pain specialist, physician | Physician, physical therapist, dentist if jaw signs are present | Physician or neurologist |
The key point is overlap. A person can have migraine and TMD. A person can have tension headache and jaw clenching. Jaw pain can also act as a trigger or amplifier for an existing headache condition.
How do you know if a headache is coming from your jaw?
You cannot know for sure without a proper evaluation. But you can look for clues.
A headache may involve the jaw if it:
- gets worse with chewing, clenching, yawning, or talking
- appears with jaw soreness, temple tenderness, or tooth sensitivity
- starts after stressful focus work or long screen time
- is worse in the morning with jaw fatigue
- occurs with clicking, popping, locking, or limited opening
- improves when you rest the jaw or soften the chewing muscles
- appears during periods of stress, concentration, or jaw bracing
Research on headache attributed to TMD has emphasized temple-area headache that changes with jaw movement, jaw function, or parafunction. It has also described headache that can be provoked by temporalis muscle palpation or jaw movement.⁴
The goal is not to diagnose yourself. The goal is to bring better clues to the right professional.
The bruxism connection: clenching, grinding, and TMD headache
Bruxism means repeated jaw muscle activity. It can happen while you are awake, during sleep, or both.
Awake bruxism often involves clenching, bracing, pressing the teeth together, or holding the jaw muscles tight during concentration or stress.
Sleep bruxism happens during sleep and can involve rhythmic jaw muscle activity, clenching, or grinding.
Both patterns matter.
You may clench while answering emails, driving, reading, working on a deadline, lifting weights, scrolling on your phone, or trying to push through stress. You may not notice it until your temples ache, your jaw feels tired, or your teeth feel sore.
When the chewing muscles stay active too long, especially the temporalis muscle at the temples, the result can feel less like “jaw pain” and more like a headache.
Sleep bruxism can be harder to detect because you are asleep when it happens. Clues include morning jaw soreness, tooth wear, cracked dental work, morning headache, or reports of grinding sounds from a bed partner.
A mouthguard may protect teeth from wear, but it may not stop the clenching habit itself. This distinction matters. Protection is useful, but awareness and behavior change are also important, especially for daytime clenching.
The difference between awake bruxism vs sleep bruxism matters because daytime clenching and nighttime grinding may need different strategies.
For a deeper look at this pattern, read Can jaw clenching cause headaches?
Biofeedback tools such as ClenchAlert may help some people notice daytime clenching patterns in real time. When the device vibrates, the goal is not to scare you or force your jaw open. The goal is to help you notice the pattern and return to a relaxed jaw position.
A simple cue can help:
That means the lips can rest gently closed while the teeth stay slightly separated and the jaw muscles soften.
This fits naturally with the BRUX Method:
- B: Build Awareness so you notice when your jaw tightens before pain escalates
- R: Relax the Response by using breath, posture, and jaw relaxation to reduce bracing
- U: Understand Triggers by tracking stress, screen time, chewing, sleep, and pain patterns
- X: Exchange the Pattern by replacing clenching with a repeatable relaxed-jaw habit
How to track whether your headache may be jaw-related
Once you understand the possible pattern, the next step is not to diagnose yourself. The next step is to notice what makes the headache better or worse. That is where tracking helps.
Use this simple tracking table for 1 to 2 weeks.
| What to track | Why it helps |
|---|---|
| Time of day | Morning pain may suggest sleep-related patterns; afternoon pain may suggest daytime tension |
| Pain location | Temples, ears, jaw, teeth, neck, or eyes may point toward different patterns |
| Jaw soreness | Helps connect head pain with jaw muscle symptoms |
| Chewing triggers | Pain that worsens with chewing may suggest jaw involvement |
| Tooth sensitivity | May suggest clenching, grinding, or dental causes |
| Ear symptoms | Helps identify jaw-ear overlap |
| Neck stiffness | Helps identify posture or muscle-chain involvement |
| Stress level | Clenching often increases during stress |
| Screen time | Concentration and posture can increase jaw bracing |
| Sleep quality | Poor sleep can increase pain sensitivity |
| Snoring or dry mouth | May suggest sleep-disordered breathing or mouth breathing |
| Clenching episodes | Builds awareness of daytime patterns |
| What helps | Relaxation, heat, jaw rest, or posture changes may reveal clues |
Ask yourself:
Does the headache get worse when my jaw works harder or when my stress level rises?
Bring this pattern to your appointment. A clear symptom history can help your clinician decide whether the jaw, teeth, neck, sleep, or another headache condition should be evaluated first.
If your symptoms are worse when you wake up, use the morning headache checklist before your next appointment.
What you can try gently at home
Most self-care should be gentle. The goal is to reduce load on the jaw, not force it into a new position.
Low-risk strategies may include:
- choose softer foods for a short period if chewing worsens pain
- avoid chewing gum
- avoid hard, chewy foods during a flare
- avoid extreme jaw opening, such as wide yawning or large bites
- practice “lips together, teeth apart”
- use warm compresses on tense jaw muscles
- take screen breaks
- relax the jaw, tongue, shoulders, and neck
- practice slow nasal breathing if comfortable
- track clenching triggers
- stop anything that increases pain
NIDCR describes simple TMD treatments as options generally tried first, including soft foods, heat or cold, short-term over-the-counter NSAIDs when appropriate, and self-management.⁵
Do not force jaw exercises, aggressive stretching, or self-manipulation if you have locking, increasing pain, joint instability, or worsening symptoms.
When to get professional help for a TMD headache
TMD headache patterns should be evaluated when symptoms are persistent, disruptive, worsening, or unclear.
| Symptom pattern | Who to ask |
|---|---|
| Temple headache with jaw soreness | Dentist or orofacial pain specialist |
| Headache worse with chewing | Dentist or orofacial pain specialist |
| Ear pain without infection | Dentist, ENT, or physician |
| Morning headache with tooth pain | Dentist and possibly a sleep professional |
| Headache with clicking, popping, locking, or limited opening | Dentist or orofacial pain specialist |
| Headache with light sensitivity, sound sensitivity, or nausea | Physician or neurologist |
| Headache with snoring, gasping, or unrefreshing sleep | Sleep physician or qualified clinician |
Start with a dentist or orofacial pain specialist when:
- headaches occur with jaw clicking, popping, or locking
- pain worsens with chewing
- you wake with jaw soreness or tooth pain
- you notice tooth wear, cracked teeth, or jaw fatigue
- ear pain has been checked but no ear cause was found
- you have limited jaw opening
- your temples feel tender when the jaw muscles are pressed
Contact a medical doctor promptly when:
Seek urgent medical care if the headache is sudden, severe, new, worsening, or unlike your usual headache.
Also seek prompt care if headache occurs with fever, confusion, weakness, numbness, vision changes, trouble speaking, fainting, injury, unexplained weight loss, or other concerning symptoms.
Ask about a sleep evaluation when:
- you wake with headaches
- you snore
- you gasp or choke during sleep
- you wake with dry mouth
- you feel unrefreshed despite enough sleep
- you have daytime sleepiness
- you have bruxism plus signs of sleep-disordered breathing
TMD, headache, bruxism, and sleep problems often require a team approach. That team may include a dentist, physician, orofacial pain specialist, physical therapist, ENT, neurologist, or sleep medicine provider.
How professionals may evaluate a TMD headache
A good evaluation should not assume the jaw is the only cause. It should look at the whole pattern.
A professional may check:
- your medical history
- your headache history
- your dental history
- jaw opening and movement
- clicking, popping, tenderness, or locking
- chewing muscle tenderness
- tooth wear, cracked teeth, or bite changes
- signs of clenching or grinding
- sleep symptoms such as snoring, dry mouth, or morning headaches
- neck posture and range of motion
- whether referral is needed to neurology, ENT, sleep medicine, physical therapy, or orofacial pain
Imaging may be used when clinically needed, but many TMD evaluations begin with a careful history and physical examination.
Treatment options for TMD-related headache
Treatment depends on the cause, severity, and pattern. Many people start with conservative care.
Possible care options include:
- education and self-care
- jaw habit awareness training
- biofeedback for daytime clenching
- physical therapy for jaw, neck, and posture patterns
- dental splints or oral appliances when appropriate
- sleep evaluation when morning headaches, snoring, or sleep disruption are present
- stress regulation strategies
- medication when recommended by a clinician
- orofacial pain specialist care for complex or persistent symptoms
- medical headache care when migraine or another headache disorder is involved
The important distinction is this:
A mouthguard may protect teeth. It may not retrain the clenching habit.
For people with daytime clenching, awareness training, trigger tracking, biofeedback, and nervous-system regulation may be important parts of the plan.
Protection matters. Training changes the pattern.
Key takeaway
A TMD headache may feel like pain in the temples, ears, forehead, face, teeth, behind the eyes, or neck. The pain may seem like a tension headache, sinus pressure, earache, toothache, or migraine pattern.
The jaw can refer pain because the jaw joint, chewing muscles, facial nerves, head, and neck are closely connected.
The best next step is pattern recognition. Track when the pain happens, where it shows up, what makes it worse, and whether jaw symptoms appear with it. Then bring that information to a qualified dentist, physician, or orofacial pain specialist.
If your headache is severe, sudden, changing, or associated with neurological or systemic symptoms, seek medical care promptly.
FAQ
Can TMD cause headaches every day?
Yes, TMD can contribute to frequent headaches in some people, especially when jaw tension, clenching, chewing muscle pain, or neck tension are ongoing. However, daily headaches should be evaluated by a healthcare professional because many conditions can cause them.
Where is a TMJ or TMD headache usually felt?
A TMD headache is often felt in the temples, forehead, around the ears, cheeks, jaw, neck, or behind the eyes. Some people also feel tooth pain, ear fullness, or facial pressure.
Is TMJ headache the same as TMD headache?
Many people use the term TMJ headache, but TMD headache is often more accurate. TMJ refers to the jaw joint itself. TMD refers to a disorder involving the joint, chewing muscles, or related structures. In everyday language, people often use both terms to describe headache pain linked to jaw problems.
How do I know if my headache is from my jaw?
A headache may be jaw-related if it worsens with chewing, clenching, jaw movement, stress, or morning jaw soreness. Clicking, locking, limited opening, tooth wear, and temple tenderness may also suggest jaw involvement.
Can TMD feel like a migraine?
Yes, TMD pain can overlap with migraine symptoms or trigger migraine in some people. However, migraine often includes features such as throbbing pain, nausea, light sensitivity, or sound sensitivity. TMD and migraine can also occur together.
Can clenching cause TMD headaches?
Yes. Repeated clenching can overload the jaw muscles and joints. This can contribute to temple pain, jaw soreness, facial pain, tooth sensitivity, and headache-like symptoms.
Should I see a dentist or doctor for a TMD headache?
Start with a dentist or orofacial pain specialist if the headache occurs with jaw pain, clicking, locking, chewing pain, tooth wear, or clenching. See a medical doctor promptly for severe, sudden, new, worsening, or unusual headaches.
References
- National Institute of Dental and Craniofacial Research. TMD (Temporomandibular Disorders). National Institutes of Health. Accessed May 7, 2026. https://www.nidcr.nih.gov/health-info/tmd
- Gauer RL, Semidey MJ. Diagnosis and treatment of temporomandibular disorders. Am Fam Physician.2015;91(6):378-386. https://www.aafp.org/pubs/afp/issues/2015/0315/p378.html
- International Headache Society. 11.7 Headache attributed to temporomandibular disorder (TMD). The International Classification of Headache Disorders, 3rd edition. https://ichd-3.org/11-headache-or-facial-pain-attributed-to-disorder-of-the-cranium-neck-eyes-ears-nose-sinuses-teeth-mouth-or-other-facial-or-cervical-structure/11-7-headache-attributed-to-temporomandibular-disorder-tmd/
- Schiffman E, Ohrbach R, List T, et al. Diagnostic criteria for headache attributed to temporomandibular disorders. Cephalalgia. 2012;32(9):683-692. https://pmc.ncbi.nlm.nih.gov/articles/PMC4521766/
- National Institute of Dental and Craniofacial Research. Summary of treatments for temporomandibular disorders. National Institutes of Health. https://www.nidcr.nih.gov/health-info/tmd/summary-treatment-temporomandibular-disorders-tmds-text-alternative
Randy Clare is a writer, educator, and health communicator focused on making complex clinical topics easier to understand. Through The Sleep and Respiratory Scholar, he creates clear, practical content on bruxism, headache, sleep, airway health, and respiratory symptoms. He is the author of The Brux Method, President of ClenchAlert.com and host of The Clenching Chronicle Podcast, where he explores jaw tension, clenching, headaches, and behavior-based approaches to relief. His work helps readers better understand symptoms, recognize patterns, and take more informed next steps.