Last updated on April 24th, 2026 at 01:59 pm
Medically responsible content note:
This article is for education only and does not diagnose or treat medical, dental, or sleep conditions. Bruxism, jaw pain, headaches, snoring, breathing pauses, and respiratory symptoms can have multiple causes. Seek care from a qualified medical, dental, sleep, or orofacial pain professional when symptoms are persistent, worsening, severe, or disruptive.
Snoring vs. sleep apnea is an important distinction because snoring is a sound, while sleep apnea is a breathing disorder.
Snoring may be harmless in some people. It can happen during a cold, allergy flare, after alcohol use, or when sleeping on your back. But loud, frequent snoring can sometimes be a sign that the upper airway is narrowing or collapsing during sleep.
In some people, that pattern is connected to obstructive sleep apnea, a condition where the upper airway becomes blocked many times during sleep, reducing or stopping airflow. Sleep apnea can fragment sleep, lower oxygen levels, and leave you feeling tired, foggy, or unrefreshed the next day.
Is snoring a sign of sleep apnea?
Snoring can be a sign of sleep apnea, but not always. Loud snoring with gasping, choking, morning headaches, daytime sleepiness, high blood pressure, or witnessed breathing pauses should be discussed with a medical provider.
In this article, you will learn the difference between snoring and sleep apnea, which warning signs deserve attention, and when to ask about sleep testing.
Is Snoring a Sign of Sleep Apnea?
Snoring can be a sign of sleep apnea, but snoring alone does not prove that you have sleep apnea.
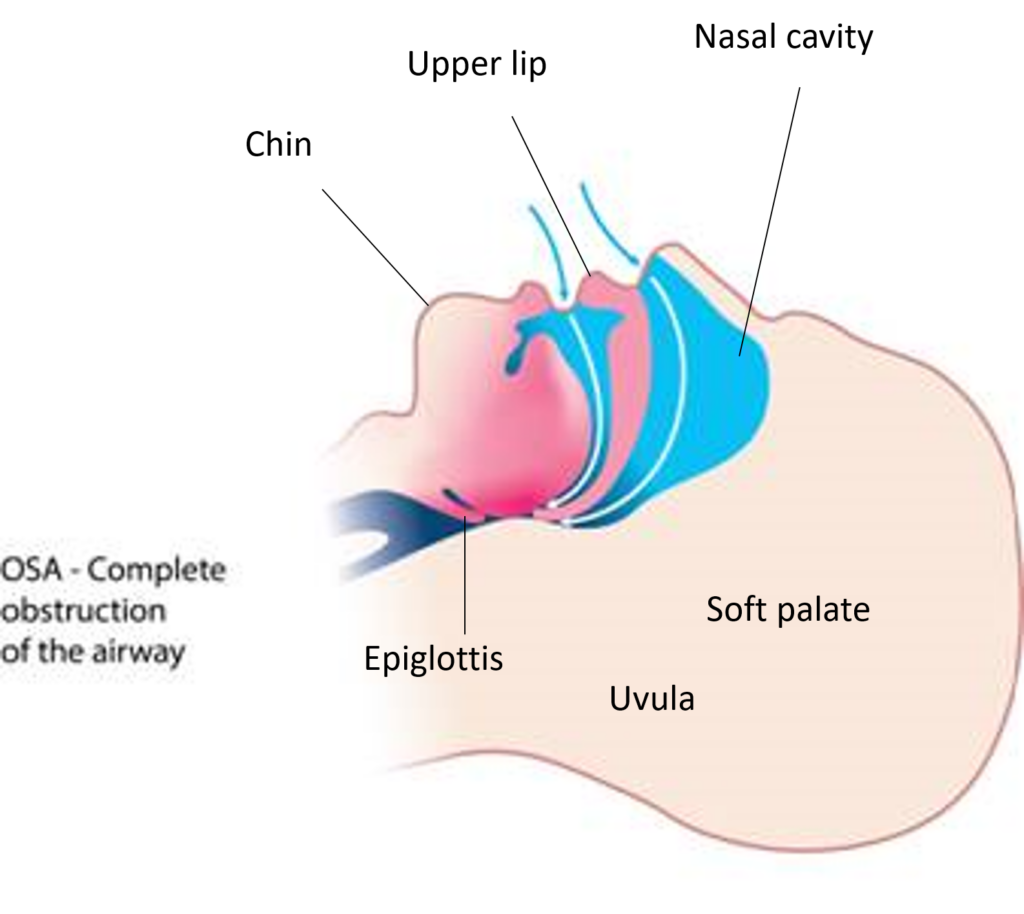
Snoring happens when air moves through a narrowed or relaxed upper airway. As air passes through the throat, soft tissues such as the soft palate, uvula, tongue, or surrounding airway structures may vibrate. That vibration creates the sound we recognize as snoring.
Obstructive sleep apnea is different. It happens when the upper airway repeatedly narrows or collapses during sleep. These breathing interruptions may reduce airflow, lower oxygen levels, and trigger brief arousals from sleep.
Many people do not remember these arousals in the morning. Instead, they may notice the effects the next day: fatigue, morning headaches, poor concentration, irritability, or feeling unrefreshed despite spending enough time in bed.
A bed partner may notice the pattern first. A person with sleep apnea may snore loudly, become quiet during a breathing pause, then gasp, choke, or snort as breathing resumes.
The important point is simple:
Snoring tells you that air is moving through a narrowed or vibrating airway. It does not tell you whether breathing is stopping, oxygen is dropping, or sleep is being repeatedly disrupted.
That is why symptoms and testing matter.
What Is the Difference Between Snoring and Sleep Apnea?
Snoring and sleep apnea can overlap, but they are not the same problem.
Snoring is usually caused by vibration. Sleep apnea involves repeated breathing disruption during sleep. A person may snore without having sleep apnea. A person may also have sleep apnea without realizing how often their breathing is being interrupted.
| Feature | Snoring | Obstructive Sleep Apnea |
|---|---|---|
| What it is | Sound from vibrating airway tissues | Repeated airway narrowing or collapse during sleep |
| Breathing interruption | Not always | Yes |
| Oxygen drops | Not necessarily | May occur |
| Common signs | Noise, bed partner disruption | Gasping, choking, fatigue, morning headaches |
| Diagnosis | Clinical evaluation may be needed if persistent | Sleep testing is required |
| Treatment | Depends on the cause | Depends on diagnosis and severity |
This difference matters because making snoring quieter does not always mean breathing is healthy. The goal is not only a quieter bedroom. The goal is safer, more restorative sleep.

Common Signs of Possible Sleep Apnea
Sleep apnea symptoms are not always obvious. Some people wake up gasping or choking. Others only know something is wrong because they feel tired, foggy, or irritable during the day.
Common signs of possible obstructive sleep apnea include:
- Loud, frequent snoring
- Gasping or choking during sleep
- Witnessed pauses in breathing
- Restless sleep
- Morning headaches
- Dry mouth on waking
- Daytime sleepiness or fatigue
- Trouble concentrating
- High blood pressure
- Waking up unrefreshed
Some people do not fit the classic stereotype. Women, younger adults, and people with smaller body types may still have sleep apnea, especially when symptoms or airway anatomy point in that direction.
Internal link callout: If you often wake with head pain, link this section to your article on morning headaches and sleep breathing problems.
Why Sleep Apnea Testing Matters
Sleep apnea cannot be diagnosed by guessing. It also cannot be ruled out by saying, “I only snore.”
A sleep study is used to measure breathing during sleep. Depending on the person and the clinical situation, this may be done with a home sleep apnea test or an in-lab sleep study. Sleep apnea testing may measure airflow, breathing effort, oxygen levels, heart rate, body position, snoring, and other sleep-related signals.
The American Academy of Sleep Medicine’s adult diagnostic testing guideline supports polysomnography or home sleep apnea testing in uncomplicated adults with signs and symptoms suggesting moderate to severe obstructive sleep apnea.
Testing helps answer important questions:
- Is sleep apnea present?
- How often is breathing disrupted?
- Are oxygen levels dropping?
- Does body position make the problem worse?
- Is treatment needed?
- Which treatment options may be appropriate?
This is especially important because treating snoring without testing can miss a more serious breathing disorder.
Internal link callout: To explain this further, link to your article on home sleep apnea testing or oxygen levels during sleep.
Myth #1: “Snoring Is Not a Big Deal”
Sometimes snoring is temporary. It may happen during a cold, an allergy flare, or after alcohol before bed. In those situations, the snoring may improve when the trigger goes away.
But loud, regular snoring should not be ignored.
The concern is not just the sound. The concern is what the sound may represent. Snoring can be a clue that the upper airway is narrowing during sleep. If that narrowing becomes severe enough to disrupt breathing, the issue may be obstructive sleep apnea.
Untreated sleep apnea can affect more than sleep. It may contribute to daytime fatigue, morning headaches, poor concentration, mood changes, high blood pressure, and cardiovascular strain.
It may also affect the bed partner, who may lose sleep because of the noise, worry, or repeated awakenings.
A useful question is not simply:
Do I snore?
A better question is:
Is my snoring part of a larger sleep-breathing problem?
That question cannot be answered by sound alone. If snoring is frequent, loud, or paired with other symptoms, it is worth discussing with a medical provider.
Myth #2: “There Is Nothing You Can Do About Snoring”
Many people live with snoring for years because they assume it is just part of who they are. That belief can keep them from taking steps that may improve sleep quality, airway health, and bed partner sleep.
The right approach depends on the cause.
For some people, snoring may improve with simple changes. These may include avoiding alcohol close to bedtime, treating nasal congestion, sleeping on the side instead of the back, improving sleep routines, or working toward a healthier weight when weight is a contributing factor.
For others, snoring may require a more structured medical or dental approach.
If snoring is related to obstructive sleep apnea, treatment may include positive airway pressure therapy, oral appliance therapy, positional therapy, medical weight management, nasal or airway evaluation, or other interventions recommended by a qualified clinician. NHLBI lists treatment options for sleep apnea that may include lifestyle changes, positive airway pressure, oral devices, surgery, and other approaches depending on the patient.
The most important step is diagnosis first.
A person should not assume that a mouthguard, snoring device, or dental appliance is appropriate without understanding whether sleep apnea is present. Snoring treatment and sleep apnea treatment may overlap, but they are not always the same clinical problem.
Myth #3: “Sleep Apnea Only Affects People Who Are Overweight”
Excess body weight is a well-known risk factor for obstructive sleep apnea, but it is not the only risk factor.
This myth can keep people from getting tested.
Sleep apnea can affect people of different body types. Airway anatomy, jaw structure, tongue position, neck size, age, sex, family history, nasal obstruction, smoking, alcohol use, certain medications, and medical conditions can all influence risk.
Some people with sleep apnea do not match the common stereotype. They may be active, thin, young, or unaware that their sleep is being disrupted. Others may think they are tired because of stress, work, parenting, aging, or poor sleep habits.
Women may also be under-recognized because their symptoms are not always described in the classic way. Instead of reporting loud snoring or obvious gasping, some may report fatigue, insomnia, headaches, mood changes, or poor-quality sleep.
The question is not:
Do I look like someone with sleep apnea?
The better question is:
Are there signs that my breathing is being disrupted during sleep?
If the signs are there, body type should not be used as a reason to dismiss the possibility of sleep apnea.
Quick Checklist: When Snoring May Need Medical Attention
Snoring may deserve medical attention when it happens with:
- Gasping or choking during sleep
- Pauses in breathing noticed by a bed partner
- Morning headaches
- Dry mouth on waking
- Daytime fatigue or sleepiness
- High blood pressure
- Restless sleep
- Poor concentration
- Waking up unrefreshed
If several of these signs are present, ask a medical provider whether sleep apnea testing is appropriate.
Internal link callout: Link this checklist to a related article on sleep apnea symptoms or when to ask your doctor about sleep testing.
What Should You Do If You Snore?
If you snore, the next step depends on the pattern.
If you snore only once in a while during a cold, allergy flare, or after drinking alcohol, watch the pattern. Occasional snoring may improve when the trigger resolves.
If you snore most nights, ask your bed partner what they notice. Do they hear gasping, choking, pauses in breathing, or sudden snorts? Do they notice that you seem restless or that your breathing changes during the night?
If you wake up with morning headaches, dry mouth, or heavy fatigue, take those symptoms seriously. They may be clues that your sleep is being disrupted.
If someone has seen you stop breathing during sleep, ask your doctor whether a sleep study is appropriate.
If sleep apnea is diagnosed, talk with your healthcare provider about treatment options. These may include CPAP, oral appliance therapy, positional therapy, lifestyle changes, airway evaluation, or a combination of approaches.
The safest next step is not guessing. It is understanding what is happening during sleep.
Snoring and Sleep Apnea Treatment Options
Treatment should be based on the diagnosis, severity, symptoms, anatomy, and patient preferences.
Positive airway pressure therapy may be recommended when the airway repeatedly collapses during sleep. CPAP and related devices use air pressure to help keep the airway open.
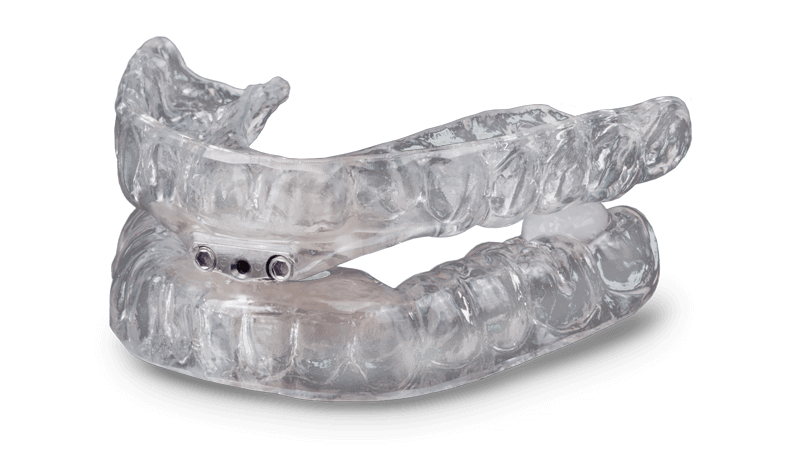
Oral appliance therapy may be considered for some patients with snoring or obstructive sleep apnea, especially when the problem involves jaw position, tongue position, or airway narrowing behind the tongue. The AASM and AADSM guideline recommends that sleep physicians consider prescription of oral appliances for adults with obstructive sleep apnea who are intolerant of CPAP or prefer alternate therapy.
Lifestyle changes may help selected patients. These may include weight management, alcohol reduction, smoking cessation, side sleeping, and improving nasal breathing.
Medical or surgical evaluation may be needed when nasal obstruction, enlarged tonsils, airway anatomy, or other structural issues contribute to the problem.
Follow-up testing is important because symptom improvement does not always prove that breathing has normalized. Feeling better matters, but objective follow-up can help confirm whether treatment is working.
Sleep apnea is not just about noise. It is about airflow, oxygen, sleep fragmentation, and health risk. That is why treatment should be guided by qualified medical and dental professionals.
Internal link callout: Link this section to your article on oral appliance therapy for sleep apnea or Randy’s personal Silent Nite sleep apnea review, if you want a first-person experience pathway.
When to Talk to a Doctor About Snoring
You should consider speaking with a medical provider if you or your bed partner notices:
- Loud snoring most nights
- Breathing pauses during sleep
- Gasping, choking, or snorting awake
- Morning headaches
- Excessive daytime sleepiness
- High blood pressure
- Waking up tired despite enough sleep
- Difficulty concentrating
- Restless sleep
- Dry mouth in the morning
If any of these symptoms happen regularly, especially with loud snoring or witnessed breathing pauses, ask whether a sleep study is appropriate.
A primary care provider, sleep physician, ENT physician, or qualified dental sleep medicine provider may be part of the care pathway, depending on the symptoms and diagnosis.
The important thing is not to ignore the pattern.
Final Takeaway
Snoring is common, but frequent loud snoring should not be dismissed.
In some people, snoring is simply vibration in a narrowed airway. In others, it may be a sign of obstructive sleep apnea. The difference matters because sleep apnea can affect oxygen levels, sleep quality, daytime function, cardiovascular health, and overall well-being.
Remember the three myths:
Snoring is not always harmless.
There are treatment options.
Sleep apnea can affect people of many body types.
If snoring is paired with gasping, choking, morning headaches, daytime fatigue, high blood pressure, or witnessed breathing pauses, talk with a medical provider about whether sleep testing is appropriate.
A quieter night is helpful. A healthier breathing pattern during sleep is the real goal.
FAQ About Snoring and Sleep Apnea
Is snoring always a sign of sleep apnea?
No. Snoring can happen without sleep apnea, especially during congestion, allergy flares, alcohol use, or back sleeping. However, loud and frequent snoring should be taken seriously when it happens with gasping, choking, daytime fatigue, morning headaches, high blood pressure, or witnessed pauses in breathing.
How do I know if my snoring is sleep apnea?
You cannot know for sure from sound alone. Snoring may suggest airway narrowing, but sleep apnea requires proper evaluation and testing. If your snoring is loud, frequent, or paired with choking, gasping, daytime sleepiness, morning headaches, or witnessed pauses in breathing, ask a medical provider whether a sleep study is appropriate.
Can you have sleep apnea without loud snoring?
Yes. Some people with sleep apnea do not report loud snoring, especially if they sleep alone or do not know what happens during the night. Daytime fatigue, morning headaches, dry mouth, poor concentration, mood changes, and high blood pressure may still be clues.
What is the difference between snoring and obstructive sleep apnea?
Snoring is the sound of airway tissues vibrating as air moves through a narrowed space. Obstructive sleep apnea involves repeated airway narrowing or collapse that disrupts breathing during sleep. Snoring may be one symptom of sleep apnea, but snoring alone does not confirm the diagnosis.
When should I get tested for sleep apnea?
Ask about testing if snoring is loud, frequent, or paired with gasping, choking, morning headaches, daytime sleepiness, high blood pressure, or witnessed pauses in breathing. A sleep study can help determine whether sleep apnea is present and how severe it may be.
Can a dentist treat snoring or sleep apnea?
A dentist trained in dental sleep medicine may help some patients with oral appliance therapy. However, sleep apnea should be diagnosed by a qualified medical provider first. Oral appliances are not the same as over-the-counter mouthguards and should be monitored as part of a proper treatment plan.
Can losing weight stop snoring or sleep apnea?
Weight loss may help some people when excess weight contributes to airway narrowing, but it is not a guaranteed cure. Sleep apnea can also be influenced by anatomy, age, jaw structure, nasal obstruction, medications, alcohol use, and other factors. Treatment should be based on diagnosis and follow-up.
Is loud snoring dangerous?
Loud snoring is not always dangerous, but it can be a warning sign. The concern is higher when loud snoring happens with gasping, choking, breathing pauses, morning headaches, daytime fatigue, or high blood pressure. In those cases, sleep apnea should be considered.
References
- National Heart, Lung, and Blood Institute. Sleep Apnea. Updated January 9, 2025.
- Kapur VK, Auckley DH, Chowdhuri S, et al. Clinical practice guideline for diagnostic testing for adult obstructive sleep apnea. J Clin Sleep Med. 2017;13(3):479-504.
- National Heart, Lung, and Blood Institute. Sleep Apnea Treatment. Updated January 9, 2025.
- Ramar K, Dort LC, Katz SG, et al. Clinical practice guideline for the treatment of obstructive sleep apnea and snoring with oral appliance therapy. J Clin Sleep Med. 2015;11(7):773-827.
Randy Clare is a writer, educator, and health communicator focused on making complex clinical topics easier to understand. Through The Sleep and Respiratory Scholar, he creates clear, practical content on bruxism, headache, sleep, airway health, and respiratory symptoms. He is the author of The Brux Method, President of ClenchAlert.com and host of The Clenching Chronicle Podcast, where he explores jaw tension, clenching, headaches, and behavior-based approaches to relief. His work helps readers better understand symptoms, recognize patterns, and take more informed next steps.





