Last updated on April 25th, 2026 at 07:09 am
Medically responsible content note:
This article is for education only and does not diagnose or treat medical, dental, or sleep conditions. Bruxism, jaw pain, headaches, snoring, breathing pauses, and respiratory symptoms can have multiple causes. Seek care from a qualified medical, dental, sleep, or orofacial pain professional when symptoms are persistent, worsening, severe, or disruptive.
What my experience taught me about oral appliance therapy, home sleep testing, and outcome verification
For more than 20 years, I have worked in sleep-disordered breathing, dental sleep medicine, and sleep therapy. I have spent years talking with dentists, dental teams, physicians, and patients about snoring, daytime sleepiness, poor sleep quality, and the consequences of untreated obstructive sleep apnea.
Over time, I developed a quiet assumption. I found myself wondering how some people could miss the signs. How could someone be tired every day, snore regularly, and still not realize that something serious might be affecting their sleep?
Then I became that person.
I started falling asleep at my desk in the afternoon. Even more concerning, I noticed myself closing my eyes while driving home. That was dangerous, and it forced me to take my own symptoms more seriously. I knew I needed evaluation and treatment. I hoped an oral appliance would be enough. If not, I was prepared to consider CPAP.
What surprised me most was this: even with my background in sleep medicine, I still could not accurately judge the severity of my own obstructive sleep apnea without a sleep test. That insight is the real reason I am sharing this story. In my view, symptoms matter, comfort matters, and patient experience matters, but objective outcome verification matters more.
Even Sleep Experts Can Miss Their Own Obstructive Sleep Apnea
By the time I decided to act, the pattern was obvious. I was middle-aged, a moderate snorer, increasingly sleepy, and no longer functioning at the level I expected from myself. My energy was dropping, and my daytime alertness was becoming less reliable.
As a first step, I completed the STOP-Bang questionnaire, which is commonly used as a screening tool for obstructive sleep apnea risk. I scored 5 out of 8, placing me in a high-risk category. That result was useful, but it was not enough. It told me I needed more information. It did not tell me how severe the problem was or what the right treatment path would be.

That is one of the limitations of screening tools. They can point you in the right direction, but they do not replace objective testing. In my case, the questionnaire helped confirm that I should look deeper, but it did not answer the question that mattered most: how much obstructive sleep apnea did I actually have?
Want to understand the condition more clearly? Click here to learn more about what obstructive sleep apnea is.
Why I Took a Home Sleep Test for Suspected Sleep Apnea
Once I recognized that screening was not enough, I moved to home sleep testing. I wanted objective data, not just impressions. That decision reflected something I have believed for years in dental sleep medicine: if you want real answers, you need measurable information.
Home sleep testing offered a practical way to evaluate my condition in a familiar environment. It also allowed me to assess the severity of my sleep-disordered breathing before beginning treatment. That was important because I did not want to rely on daytime symptoms, snoring, or personal intuition alone.
This is a point worth emphasizing for both patients and clinicians. Many people assume they can estimate severity based on how they feel. In my experience, that is not reliable enough. I was surprised that even as experienced with sleep as I am, I still was unable to judge the severity of my OSA without a sleep test. That one realization changed the way I think about my own case and reinforced what I already teach others.
If your symptoms sound familiar, click here to review the signs you may need a sleep study
How I Used a NOX T3 Home Sleep Test and EMG Monitoring
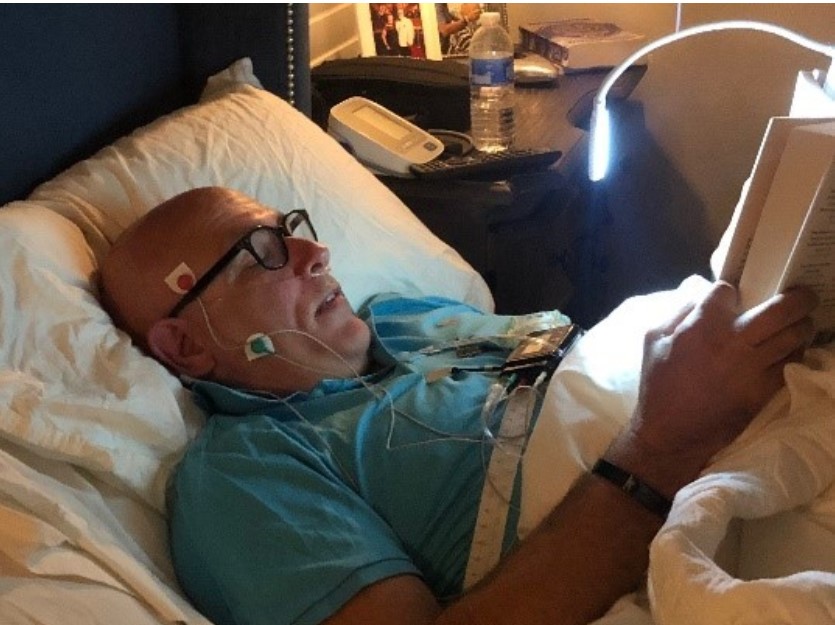
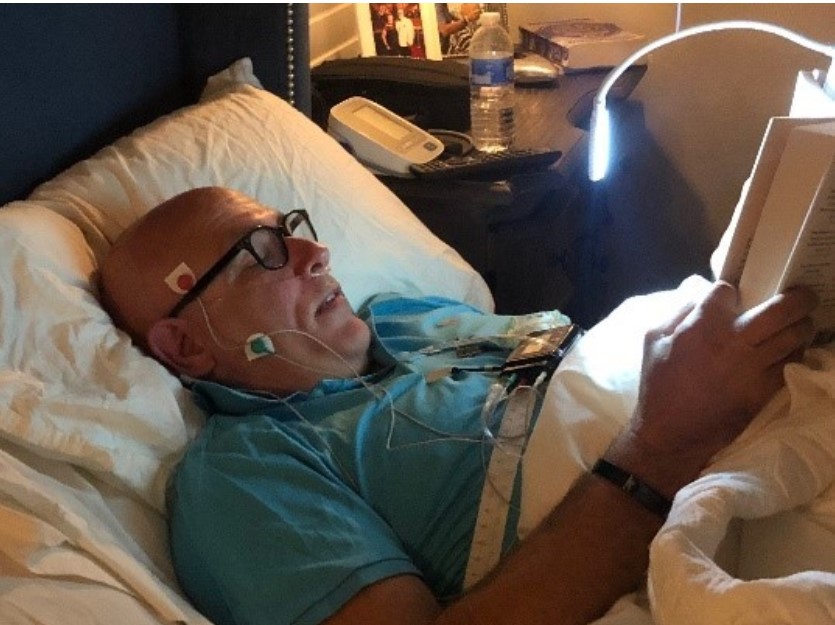
To evaluate my sleep objectively, I used a NOX T3 from NOX Medical for a home sleep study. Because of my interest in the relationship between airway problems and parafunctional activity, I also added EMG monitoring. Specifically, I placed EMG leads on my masseter and temporalis muscles to assess bruxism-related muscle activity during sleep. The study was scored using the scoring algorithm in the NOX software.
The test setup included the expected home sleep testing components, including the RIP belts, nasal cannula, and Nonin Wristox2 pulse oximeter. Fortunately, the study went smoothly. The leads stayed in place, and the recording was successful. I did wake earlier than usual, so the study was shorter than I would have preferred, but it still provided valuable information.
That combination of respiratory monitoring and EMG observation gave me a broader view of what was happening during sleep. In my opinion, this kind of careful evaluation helps support better clinical decision-making, especially when sleep-disordered breathing and bruxism may overlap.
What My First Sleep Study Revealed About My Obstructive Sleep Apnea
My initial home sleep study showed an AHI in the high mild range, close to the threshold for moderate obstructive sleep apnea.
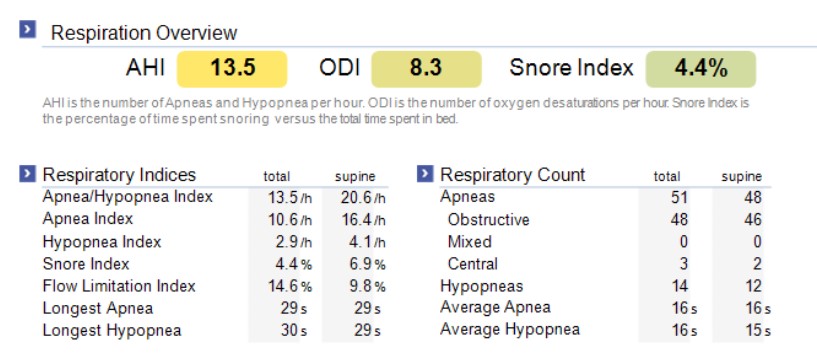
That result mattered for two reasons.
First, it confirmed that my symptoms were tied to objectively measurable sleep-disordered breathing. I was not simply tired from stress or getting older. There was a real physiological problem to address.
Second, it reminded me that even people with substantial experience in this field can have blind spots when evaluating themselves. I knew enough to recognize that something was wrong, but I did not know enough from symptoms alone to accurately judge the degree of the problem.
That is why this article is not just a product review. It is also a reminder that expertise does not eliminate the need for diagnostics. If anything, it should increase our respect for them.
Why I Chose a Silent Nite SL Oral Appliance
Once the test confirmed that treatment was warranted, I scheduled a dental appointment to have a Silent Nite SL made. This mandibular advancement device is fabricated by Glidewell Dental Lab in Irvine, California. The principle behind this kind of therapy is straightforward: by advancing the mandible during sleep, the appliance can help improve upper airway patency in appropriate patients.
For me, this was a logical treatment option. My obstructive sleep apnea was mild, though close to moderate, and I wanted to see whether a custom oral appliance could reduce breathing events and improve my sleep quality. I also chose a second appliance for travel so I could maintain the routine consistently when away from home.
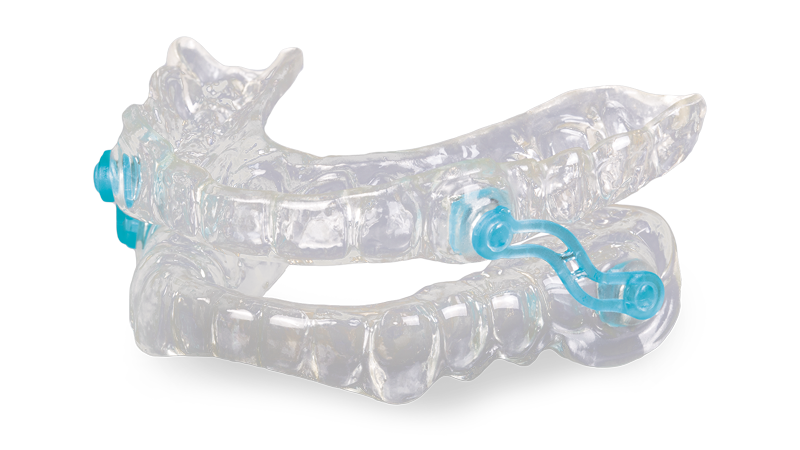
The Silent Nite SL came with 25 mm connectors in place, which served as my starting position. Because shorter connectors increase mandibular advancement, the device offered a simple titration pathway that allowed me to make controlled changes over time. That adjustability is one of the practical strengths of oral appliance therapy when it is used thoughtfully and followed carefully.
Why Early Improvement Did Not Mean I Was Fully Treated
When I first started wearing the appliance, I thought I was doing well almost immediately. For several nights, I felt encouraged. I thought I was sleeping better and assumed I had found the answer quickly.
Then my wife told me I was still snoring heavily.
That moment was important because it exposed one of the biggest clinical traps in oral appliance therapy: early subjective improvement can be misleading. A patient may feel better before the airway is adequately treated. The appliance may be comfortable, but comfort is not the same thing as therapeutic success. A bed partner may notice continued snoring or breathing noise even when the patient believes everything is under control.
If I had stopped with my first impression, I might have assumed success too soon. Instead, I learned again that symptom improvement is meaningful, but it is not the same thing as verified treatment.
How Titration Changed My Sleep Apnea Results
Because I was still snoring, I advanced my jaw by 1 mm by changing from the 25 mm connectors to the 24 mm connectors. I tolerated that change well. Some patients need time to adapt even to a small shift in mandibular position, but in my case the adjustment was easy.
Still, I did not want to assume it was working simply because it felt acceptable. I wanted data.
So I repeated the home sleep test. The follow-up study showed real improvement. My AHI dropped to 7.1, nearly half of the original level, and snoring decreased from 4.4% of the night to 1.7%. That was a very meaningful response, but it was not the endpoint I wanted. I was improved, but not yet fully normalized.
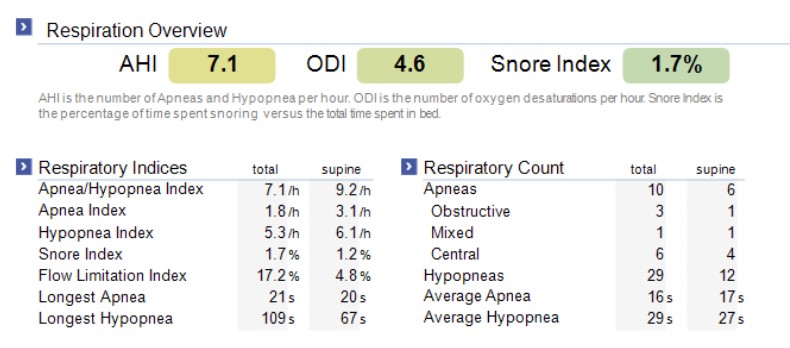
At that stage, many patients and clinicians would be tempted to stop. The appliance was helping. I felt better. The numbers were better. But better is not always enough. That is exactly why titration and follow-up testing matter.
To see whether I could improve the outcome further, I switched to the 23 mm connectors and repeated the study again. This time, my AHI was 4.6, below the threshold of 5 that is commonly considered within the normal range. That was the objective outcome I had hoped to achieve. Interestingly, my snoring increased somewhat at that stage, which is another reminder that treatment response is not always perfectly linear. One metric may improve while another behaves differently. That is why oral appliance therapy should be judged in a balanced way, not through a single number alone.
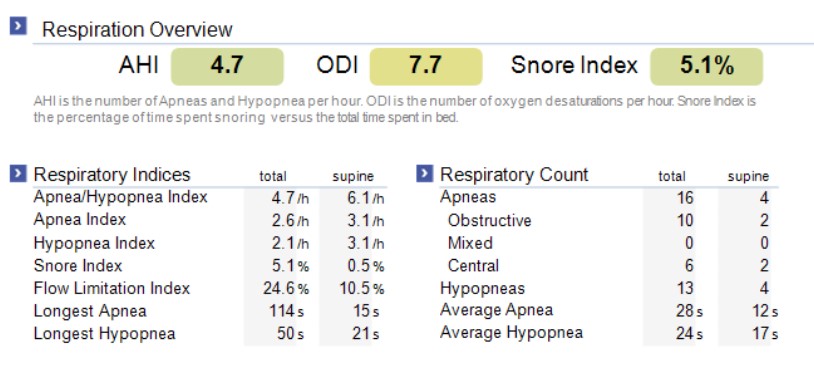
Why Outcome Verification Matters in Oral Appliance Therapy
This was the central lesson of the entire experience.
An oral appliance is not successful simply because it is comfortable. It is not successful simply because the patient likes it. It is not successful simply because the patient reports improvement. It is successful when the therapy is objectively verified and the data show that the airway is being adequately managed.
That principle matters for patients because undertreated obstructive sleep apnea still carries risk. It matters for dentists because dental sleep medicine is not just about delivering a device. It is about participating in a medical treatment pathway that includes screening, collaboration, titration, follow-up, and verification.
If oral appliances are going to be taken seriously as a treatment for obstructive sleep apnea, then outcome verification has to be part of the conversation. My own case reinforced that point in a very personal way.
What My Experience Taught Me About Dental Sleep Medicine
This experience strengthened my confidence in oral appliance therapy, but it also sharpened my view of standards of care. In my opinion, dental sleep medicine works best when it is approached with discipline. Screening matters. Appliance selection matters. Titration matters. Patient comfort matters. But none of those replace outcome verification.
This is also one reason I believe dental sleep medicine should be discussed with the seriousness it deserves. When dentists provide oral appliance therapy, they are not simply offering a dental product. They are participating in care that affects breathing, sleep quality, daytime alertness, and long-term health.
I am sharing this case for two reasons. First, I want to demonstrate that when oral appliances are used to treat obstructive sleep apnea, some form of objective follow-up is vital. Second, I want this article to reflect how I approach dental sleep medicine, sleep therapy, and sleep diagnostics. I believe in practical tools, careful thinking, and measurable results. This experience did not just confirm a diagnosis for me. It reinforced the importance of maintaining a disciplined, evidence-aware approach, even in cases that may seem straightforward at first.
Final Thoughts on Treating Obstructive Sleep Apnea With a Silent Nite SL
The Silent Nite SL proved to be a comfortable and effective therapy for me. But the most important takeaway from this experience is bigger than one appliance or one set of sleep studies.
The real lesson is this: you cannot responsibly manage obstructive sleep apnea based on guesswork.
Not on symptoms alone.
Not on comfort alone.
Not on optimism alone.
You need objective testing to understand the condition, and you need objective follow-up to confirm the result.
I believed that before this experience. Now I know it in a much more personal way.
Author note
Randy Clare has spent more than two decades working in sleep-disordered breathing, dental sleep medicine, and sleep therapy. His work focuses on oral appliance therapy, sleep diagnostics, clinical communication, and practical education for dentists, teams, and patients navigating sleep-related breathing disorders.
This article describes one person’s experience with obstructive sleep apnea, home sleep testing, EMG monitoring, and oral appliance therapy. It is for educational purposes only and should not be used as a substitute for medical or dental evaluation, diagnosis, or treatment. Care decisions for obstructive sleep apnea should be made with qualified healthcare professionals and verified with appropriate follow-up.
Randy Clare is a writer, educator, and health communicator focused on making complex clinical topics easier to understand. Through The Sleep and Respiratory Scholar, he creates clear, practical content on bruxism, headache, sleep, airway health, and respiratory symptoms. He is the author of The Brux Method, President of ClenchAlert.com and host of The Clenching Chronicle Podcast, where he explores jaw tension, clenching, headaches, and behavior-based approaches to relief. His work helps readers better understand symptoms, recognize patterns, and take more informed next steps.