Last updated on May 6th, 2026 at 08:51 am
Medically responsible content note:
This article is for education only and does not diagnose or treat medical, dental, or sleep conditions. Bruxism, jaw pain, headaches, snoring, breathing pauses, and respiratory symptoms can have multiple causes. Seek care from a qualified medical, dental, sleep, or orofacial pain professional when symptoms are persistent, worsening, severe, or disruptive.
Sleep problems do not always look like sleep problems.
Sometimes they look like morning headaches, brain fog, loud snoring, jaw tension, dry mouth, poor concentration, irritability, low energy, or the feeling that a full night in bed did not actually restore anything. Many people live with these symptoms for years without realizing that sleep itself may be part of the problem.
That is one reason sleep disorders are so often missed. A person may assume they are stressed, overworked, aging, or simply “not sleeping well.” They may blame fatigue on a busy schedule or headaches on tension. They may not know that breathing can repeatedly break down during sleep, or that insomnia, nighttime movement, or circadian disruption can quietly interfere with recovery night after night.
Sleep apnea is one of the most important sleep disorders to recognize because it can affect breathing, oxygen levels, sleep continuity, cardiovascular strain, daytime alertness, and overall quality of life. But it is not the only condition that can interfere with healthy sleep. Insomnia, restless legs syndrome, circadian rhythm sleep disorders, parasomnias, hypersomnolence disorders, and sleep-related movement disorders can all disrupt sleep in different ways.
This guide explains what sleep disorders are, how sleep apnea fits into the larger picture, what symptoms matter most, how testing works, and what treatment options may help. If your sleep leaves you tired, foggy, sore, unrested, or concerned, this is where to start.
In This Guide
- What sleep disorders are and how they disrupt sleep
- The most common sleep disorders and how they differ
- What sleep apnea is and why it affects more than snoring
- Symptoms of sleep apnea and other sleep disorders to watch for
- Who is at risk for sleep apnea and other sleep disorders
- How sleep disorders are diagnosed
- Home sleep tests vs lab studies
- Sleep apnea treatment options
- How sleep apnea can overlap with headaches, bruxism, fatigue, and more
What Sleep Disorders Are and How They Disrupt Sleep
Sleep disorders are conditions that disrupt the quality, timing, structure, or regulation of sleep. Some affect breathing, while others interfere with falling asleep, staying asleep, movement during sleep, or the body’s internal sleep-wake timing.
Healthy sleep depends on several systems working together. Breathing must remain stable. The brain must cycle through normal sleep stages. Muscles must relax and activate at the right times. The internal body clock must stay reasonably aligned with light, darkness, and daily routines. When one or more of these systems becomes unstable, sleep may become fragmented, shallow, mistimed, or physiologically stressful.
That matters because sleep is not just about how long you stay in bed. It is also about whether the body gets restorative, continuous, biologically effective sleep. A person can spend eight hours in bed and still wake up tired if sleep has been broken up by breathing events, repeated arousals, limb movements, pain, reflux, or circadian disruption.
This is why sleep disorders often hide behind everyday complaints. Fatigue may be blamed on stress. Poor focus may be blamed on overload. Mood changes may be treated as separate from sleep. Morning headaches may be handled as a pain issue without anyone asking what happened overnight. When sleep is poor often enough, the whole day can start to reflect it.
For many readers, this is the first important shift: poor sleep is not always a lifestyle problem. Sometimes it is a diagnosable sleep problem.
The Most Common Sleep Disorders and How They Differ
Sleep medicine covers a wide range of conditions, but several disorders appear again and again in real life.
Sleep apnea
Sleep apnea is a disorder in which breathing repeatedly slows, narrows, or stops during sleep. Obstructive sleep apnea happens when the airway becomes too narrow or collapses. Central sleep apnea happens when breathing effort becomes unstable because the brain does not consistently send the right signals. Both can interfere with sleep quality and daytime function, though obstructive sleep apnea is far more common.
Insomnia
Insomnia involves persistent difficulty falling asleep, staying asleep, or returning to sleep after waking too early. It is not just a rough night here and there. Over time, insomnia can become a learned cycle in which worry, frustration, and hyperarousal make sleep even harder.
Restless legs syndrome and periodic limb movements
Restless legs syndrome causes an urge to move the legs, often with uncomfortable sensations that worsen during rest or later in the day. Periodic limb movements involve repetitive jerking or twitching during sleep. Both can reduce sleep continuity and leave a person feeling worn down.
Circadian rhythm sleep disorders
These disorders involve a mismatch between the body’s internal clock and the schedule a person needs to follow. Shift work disorder, delayed sleep-wake phase disorder, and jet lag are common examples. In these cases, the problem may not be a total inability to sleep, but sleeping at the wrong biological time.
Parasomnias
Parasomnias involve unusual behaviors or experiences during sleep, such as sleepwalking, night terrors, confusional arousals, or REM sleep behavior disorder. Some are more common in children. Others deserve careful attention in adults.
Hypersomnolence disorders
These disorders cause excessive daytime sleepiness that goes beyond ordinary tiredness. Narcolepsy and idiopathic hypersomnia fall into this category. A person may feel overwhelmingly sleepy even when trying to get enough sleep.
Sleep-related movement disorders
Some disorders involve repetitive or abnormal movement during sleep. Sleep bruxism belongs in this broader discussion, especially when it overlaps with arousals, pain, airway issues, or unrestorative sleep.
If you plan to build cluster content from this page, this section naturally supports deeper articles on insomnia vs sleep apnea, restless legs syndrome symptoms, shift work disorder and sleep, and sleep bruxism and sleep quality.
What Sleep Apnea Is and Why It Affects More Than Snoring
Sleep apnea is a sleep-related breathing disorder in which airflow repeatedly decreases or stops during sleep. These breathing disruptions can fragment sleep, lower oxygen levels, and affect daytime energy, concentration, and overall health.
Sleep apnea matters because it does more than create noise at night. It can interfere with recovery, strain the body’s stress response, and leave a person feeling unrested even after what looks like a full night of sleep.
Obstructive sleep apnea
Obstructive sleep apnea, or OSA, happens when the upper airway narrows or collapses during sleep. Muscle tone naturally decreases when you sleep. In some people, that drop in tone combines with anatomy, soft tissue crowding, body position, nasal resistance, or other factors that make the airway unstable.
When the airway narrows enough, airflow is reduced or blocked. Many of these events end with a brief arousal. A person may gasp, snort, shift, tense up, or wake partly without remembering it the next morning.
This cycle can repeat over and over all night long.
Central sleep apnea
Central sleep apnea, or CSA, is different. In central sleep apnea, breathing pauses occur because the brain does not consistently maintain the signal to breathe. This pattern is less common than OSA and is often associated with more complex medical or neurologic factors.
Why sleep apnea affects the whole day
Sleep apnea is not just snoring with a medical label. Repeated breathing disruption can trigger oxygen fluctuations, frequent arousals, stress-response activation, heart rate changes, and broken sleep architecture. Over time, that can affect energy, mood, focus, blood pressure regulation, pain sensitivity, and how restored a person feels during the day.
The core problem happens at night, but the consequences often show up after the sun is up.
Symptoms of Sleep Apnea and Other Sleep Disorders to Watch For
Common symptoms of sleep apnea include loud snoring, witnessed pauses in breathing, gasping during sleep, dry mouth, morning headaches, daytime fatigue, brain fog, and nonrestorative sleep.
Many people expect sleep disorders to feel obvious. In reality, the signs are often scattered, gradual, and easy to normalize.
Nighttime symptoms
Common nighttime symptoms of sleep apnea and other sleep disorders include:
- loud snoring
- gasping or choking during sleep
- witnessed pauses in breathing
- frequent waking
- dry mouth on waking
- night sweats
- restless sleep
- frequent urination at night
- reflux during sleep
- teeth grinding or jaw tension during the night
Insomnia may show up as lying awake for long stretches, waking repeatedly, or waking too early and being unable to return to sleep.
Movement-related disorders may involve kicking, twitching, repeated limb movements, or a strong urge to move the legs at night.
Circadian rhythm disorders often show up as being unable to fall asleep at the desired time or feeling forced to stay awake when the body is biologically primed for sleep.
Daytime symptoms
The daytime symptoms are often what push people to start searching for answers. These may include:
- fatigue
- excessive sleepiness
- brain fog
- poor memory
- low motivation
- morning headaches
- jaw soreness
- irritability
- reduced productivity
- decreased exercise recovery
- anxiety symptoms
- depressed mood
- trouble staying mentally sharp
Many people do not describe this as sleepiness. They describe it as feeling flat, unrefreshed, foggy, or not fully functional.
Common signs people brush off
Some of the most important clues do not sound dramatic:
- needing caffeine to get going
- waking with a dry mouth
- falling asleep in front of the TV
- feeling sleepy while driving
- relying on multiple alarms
- waking with temple pain or facial tension
- hearing from a bed partner that you snore, stop breathing, or seem restless
- sleeping for many hours but still feeling poorly restored
These signs do not prove someone has sleep apnea, but they should not be ignored.
How symptoms differ by disorder
Sleep apnea often shows up as snoring, gasping, breathing pauses, dry mouth, morning headaches, and daytime sleepiness or fatigue. Insomnia more often shows up as difficulty sleeping despite having the chance to sleep. Circadian rhythm disorders usually involve mistimed sleep rather than a total inability to sleep. Restless legs syndrome tends to involve an urge to move the legs and discomfort during rest. Parasomnias involve unusual sleep behaviors.
The challenge is that overlap is common. A person may have more than one issue affecting sleep at the same time.
Who Is at Risk for Sleep Apnea and Other Sleep Disorders
Risk factors do not create a diagnosis on their own, but they can raise suspicion.
Risk factors for obstructive sleep apnea
Risk factors for OSA include excess weight, older age, family history, larger neck circumference, upper airway anatomy, nasal obstruction, alcohol use near bedtime, sedating medications, smoking, and hormonal changes such as menopause. OSA can also occur in people who do not fit the classic stereotype, which is one reason it is underdiagnosed.
Risk factors for insomnia
Insomnia is often associated with stress, anxiety, depression, chronic pain, hyperarousal, irregular schedules, poor sleep conditioning, medication effects, and medical illness. For many people, the problem becomes self-reinforcing over time.
Risk factors for other sleep disorders
Restless legs syndrome may be linked to iron deficiency, pregnancy, kidney disease, and neurologic factors. Circadian rhythm disorders are common in shift workers and people with unstable schedules. Parasomnias may be worsened by sleep deprivation, stress, alcohol, fever, certain medications, or coexisting sleep disorders. Hypersomnolence disorders involve more specialized neurologic mechanisms and require careful evaluation.
Sleep disorders in children
Children can have sleep disorders too, and the signs may not look like adult sleepiness. Snoring, mouth breathing, restless sleep, behavior problems, hyperactivity, irritability, poor school performance, and enlarged tonsils or adenoids can all point toward sleep-related problems in children.
How Sleep Disorders Can Affect Mood, Focus, Pain, and Overall Health
Sleep disorders do not only make people tired. They can change how the brain functions, how the body recovers, and how manageable daily life feels.
Effects on attention and daily performance
Broken or shallow sleep can impair concentration, memory, reaction time, decision-making, and emotional regulation. People may become more forgetful, more irritable, less productive, and less resilient. Even mild but repeated sleep disruption can make ordinary tasks feel harder.
Effects on cardiovascular and metabolic health
Sleep apnea in particular has been associated with cardiovascular strain, blood pressure problems, and metabolic disruption. Repeated oxygen changes, sleep fragmentation, and stress-response activation help explain why the disorder matters medically, not just symptomatically.
Effects on pain and physical recovery
Poor sleep can lower pain tolerance and make muscle tension, headaches, facial soreness, and chronic pain patterns feel worse. For some people, morning headaches or jaw soreness are among the first signs that nighttime recovery is not going well.
Effects on quality of life
Snoring can disrupt a bed partner’s sleep. Daytime fatigue can affect work, parenting, exercise, and motivation. Brain fog can make a person feel unlike themselves. The impact may build slowly, but it is often substantial.
How Sleep Disorders Are Diagnosed
Diagnosis begins with careful history and the right testing for the problem being considered.
A clinician may ask about snoring, breathing pauses, waking patterns, bedtime routines, daytime sleepiness, headaches, dry mouth, medication use, caffeine, alcohol, shift work, pain, mood symptoms, and what a bed partner has observed. Screening tools such as the Epworth Sleepiness Scale, STOP-BANG questionnaire, symptom inventories, and sleep logs may help identify risk.
From there, the evaluation depends on the suspected disorder.
Sleep apnea usually requires objective testing. Insomnia may rely more heavily on clinical history and behavioral pattern assessment. Circadian rhythm disorders may call for sleep logs, schedule analysis, and sometimes actigraphy. Movement disorders, parasomnias, and hypersomnolence disorders may require more specialized testing or full overnight sleep studies.
In practice, sleep disorders may be evaluated by sleep physicians, pulmonologists, neurologists, ENT specialists, primary care clinicians, and other trained professionals. When oral appliance therapy is being considered for sleep apnea, dental sleep medicine may become part of the treatment pathway as well.
Sleep Apnea Testing Explained: Home Sleep Tests vs Lab Studies
Sleep apnea is diagnosed through clinical evaluation and objective testing, usually with either a home sleep apnea test or an in-lab sleep study. Diagnosis is based on breathing patterns during sleep, not snoring alone.
What a home sleep apnea test can show
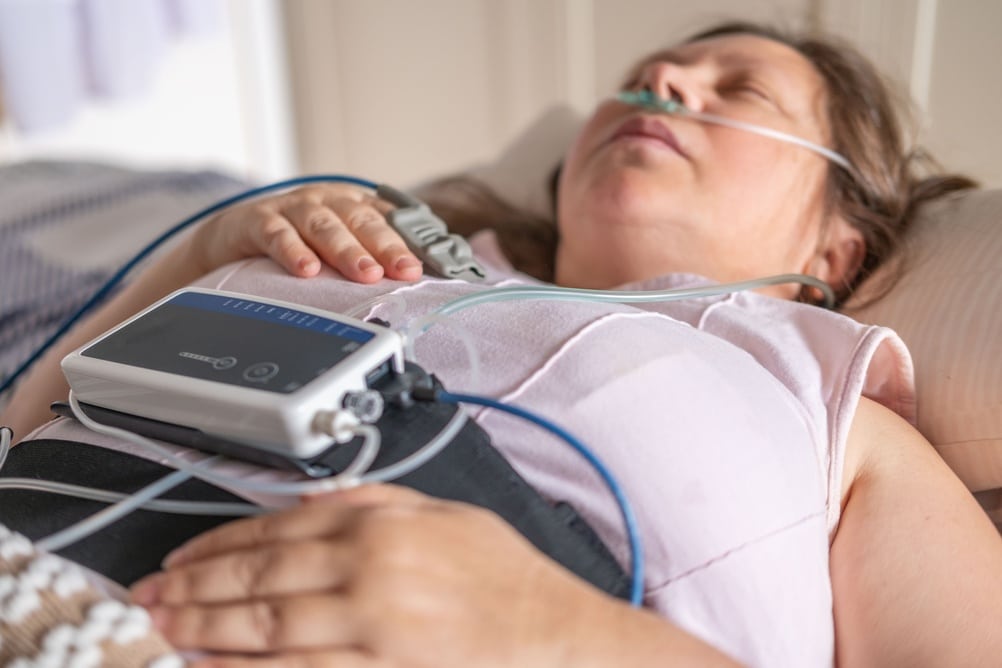
A home sleep apnea test measures breathing-related abnormalities during sleep, such as airflow changes, breathing effort, oxygen levels, and pulse-related signals. It is commonly used to evaluate suspected obstructive sleep apnea.
A home sleep apnea test focuses primarily on breathing-related abnormalities during sleep. It is often a practical option when obstructive sleep apnea is strongly suspected and the clinical picture is relatively straightforward.
The main advantage is convenience. The main limitation is that it does not capture the full range of physiologic information that a lab study can.
What an in-lab sleep study can show
An in-lab polysomnogram provides a much more complete picture of sleep. It typically measures brain waves, sleep stages, eye movements, muscle activity, airflow, respiratory effort, oxygen levels, heart rhythm, and often limb movements.
This makes lab testing especially valuable when the clinical picture is more complex or when central sleep apnea, parasomnias, limb movement disorders, or multiple overlapping sleep problems are being considered.
Home testing vs lab testing
A home sleep test focuses mainly on breathing-related problems, while a lab sleep study measures a wider range of signals including brain waves, sleep stages, airflow, oxygen levels, heart rhythm, and limb movements.
Home testing is simpler and more convenient. In-lab testing is more comprehensive. The right choice depends on the person’s symptoms, risk profile, medical background, and the disorder being evaluated.
What happens after testing
Once results are reviewed, the next step is diagnosis, treatment planning, and follow-up. Testing is not the finish line. It is the beginning of a more informed treatment decision.
What Sleep Apnea Severity Means and Why AHI Is Not the Whole Story
AHI, or apnea-hypopnea index, is one of the most common ways sleep apnea severity is described. It reflects how many breathing events occur per hour of sleep or recorded time, depending on the type of test.
AHI is useful, but it does not tell the whole story.
Two people with the same AHI may feel very different. One may have severe fatigue, morning headaches, and poor concentration. Another may have fewer obvious symptoms. That is because disease burden is influenced by more than event count alone.
Oxygen patterns matter. Repeated oxygen drops may place more strain on the body than brief, lighter events. Sleep fragmentation matters too. A person may feel awful because sleep is repeatedly interrupted, even if the event count does not look dramatic at first glance. Sleep stage and body position matter as well. Some people have more severe breathing disruption during REM sleep or while lying on their back.
This is why a thoughtful evaluation looks beyond a single number. Symptoms, oxygen burden, arousals, sleep architecture, positional effects, comorbid conditions, and treatment response all help define how meaningful the disorder is in real life.
Sleep Apnea Treatment Options: CPAP, Oral Appliances, and More
Treatment options for sleep apnea may include CPAP therapy, oral appliance therapy, positional therapy, weight management, lifestyle changes, and sometimes surgery. The right treatment depends on the type and severity of sleep apnea and the patient’s overall health.
Sleep apnea treatment should fit both the disorder and the person living with it. The best treatment is not just the one that works in theory. It is the one that can be used consistently and monitored appropriately.
CPAP therapy
Continuous positive airway pressure, or CPAP, uses pressurized air to help keep the airway open during sleep. It is often highly effective for obstructive sleep apnea because it directly addresses airway collapse. For some patients, CPAP is an excellent fit. For others, comfort, mask tolerance, dryness, pressure discomfort, or routine burden can make long-term use harder.
Oral appliance therapy
Oral appliance therapy uses a custom-fitted device to help support the airway during sleep, often by repositioning the lower jaw. For selected patients, it can be a practical and effective treatment option, especially when delivered through an appropriate collaborative care model and followed objectively.
Positional therapy
Some people have worse sleep apnea when sleeping on their back. Positional therapy aims to reduce back-sleeping when position is clearly contributing to airway collapse.
Weight loss and lifestyle strategies
Weight reduction, when appropriate, can improve sleep apnea severity in some individuals. Other supportive measures may include reducing alcohol close to bedtime, treating nasal obstruction, smoking cessation, and improving sleep routines. These strategies can help, but they do not replace formal treatment when clinically significant sleep apnea is present.
Surgery and airway procedures
Some patients may be candidates for ENT evaluation or other airway procedures, particularly when anatomy is a major contributor or when other therapies are ineffective or poorly tolerated.
Combination therapy
Not every patient needs only one treatment. Some benefit from combined approaches, such as CPAP plus positional strategies, or oral appliance therapy plus broader lifestyle support.
Treatment Options for Insomnia, Restless Legs, and Other Sleep Disorders
Not every sleep complaint should be routed into a sleep apnea framework. The treatment has to match the diagnosis.
Insomnia treatment
Chronic insomnia is often treated most effectively with cognitive behavioral therapy for insomnia, or CBT-I. This approach addresses the behavioral and mental patterns that keep insomnia going. Sleep hygiene can help, but by itself it is usually not enough for persistent insomnia.
Restless legs syndrome treatment
Treatment may include iron evaluation, medication review, trigger management, and, in some cases, prescription therapy. Pattern recognition is important because symptoms often worsen in the evening or during inactivity.
Circadian rhythm disorder treatment
These disorders may respond to timed light exposure, carefully timed melatonin, schedule restructuring, and behavioral strategies designed to shift or stabilize the body clock.
Parasomnia management
Parasomnias often require attention to safety first, along with review of sleep deprivation, stress, alcohol, medications, and coexisting sleep disorders that may be contributing.
Hypersomnolence disorders
Narcolepsy and related conditions require specialized evaluation because overwhelming daytime sleepiness can have several different causes and deserves a careful differential diagnosis.
What to Do If You Think You Have a Sleep Disorder
If your sleep seems tied to headaches, fatigue, snoring, dry mouth, jaw tension, brain fog, poor concentration, or daytime sleepiness, it is worth looking closer.
Start by watching for patterns. Do you wake unrefreshed even after enough time in bed? Has anyone noticed you snore, stop breathing, gasp, grind your teeth, or seem unusually restless? Do you wake with headaches or a dry mouth? Do you feel sleepy in passive situations or mentally dull even after sleeping?
A short symptom log can help. Track your bedtime, wake time, awakenings, naps, caffeine use, alcohol use, morning symptoms, daytime sleepiness, and anything a bed partner notices. Even one or two weeks of notes can make a clinical conversation much more useful.
When you seek evaluation, bring the pattern with you. Helpful questions include:
- Could my symptoms point to sleep apnea or another sleep disorder?
- What kind of testing makes sense in my case?
- If a sleep disorder is found, what are the treatment options?
- How will treatment be followed and verified?
The goal is not simply to name the problem. It is to understand what is disturbing sleep and what can realistically improve it.
How Sleep Apnea Can Overlap With Headaches, Bruxism, Fatigue, and More
Sleep apnea often overlaps with the very symptoms that send people searching for help.
Morning headaches
Morning headaches can be linked to sleep-disordered breathing, fragmented sleep, oxygen fluctuations, jaw tension, or more than one factor at once. When headaches keep showing up in the morning, sleep belongs on the list of possible contributors.
Bruxism and jaw tension
Nighttime jaw activity and sleep-disordered breathing may overlap in some individuals. Morning facial soreness, temple tenderness, tooth wear, or jaw tension do not automatically mean sleep apnea is present, but the relationship is clinically important enough to deserve attention.
GERD and nighttime reflux
Poor sleep and nighttime reflux often travel together. Waking with throat irritation, reflux symptoms, or a sour taste may point to more than a digestive issue alone.
Mood symptoms and brain fog
Poor sleep can intensify irritability, anxiety, low mood, and mental dullness. In some people, the emotional story is only part of the picture. The other part is chronic nighttime disruption.
High blood pressure and physical strain
Sleep apnea is an important consideration in some people with stubborn blood pressure issues, especially when snoring, fatigue, and poor sleep quality are also part of the story.
Chronic fatigue and nonrestorative sleep
If you spend enough time in bed but never feel restored, sleep quality deserves just as much attention as sleep duration.
Key Takeaways on Sleep Apnea and Common Sleep Disorders
Sleep disorders are common, but they are often missed because their symptoms overlap with everyday problems like fatigue, stress, headaches, poor focus, and mood changes. Sleep apnea is one of the most important to recognize because it repeatedly disrupts breathing, sleep continuity, and recovery. But it is only one of several disorders that can interfere with restorative sleep.
Insomnia, restless legs syndrome, circadian rhythm disorders, parasomnias, hypersomnolence disorders, and sleep-related movement disorders can all affect how a person sleeps and how they function during the day. The right diagnosis depends on symptom patterns, clinical history, and, when needed, objective testing.
The good news is that sleep disorders are not just something to endure. Many are diagnosable, manageable, and treatable. If sleep leaves you tired, foggy, sore, or concerned, it is worth taking seriously.
Frequently Asked Questions About Sleep Apnea and Sleep Disorders
1. What are the most common symptoms of sleep apnea?
The most common symptoms of sleep apnea include loud snoring, witnessed pauses in breathing, gasping during sleep, dry mouth on waking, morning headaches, nonrestorative sleep, excessive daytime sleepiness, brain fog, and irritability. Some people notice mostly fatigue and poor focus rather than obvious sleepiness. Others are alerted by a bed partner who hears snoring or notices breathing pauses. Because the signs can be subtle or spread across different parts of life, sleep apnea often goes unrecognized until symptoms become hard to ignore.
2. Can you have sleep apnea without knowing it?
Yes. Many people with sleep apnea do not realize they have it because the clearest signs happen during sleep. They may not hear their own snoring or remember waking after breathing events. Instead, they may just feel exhausted, foggy, headachy, or mentally flat during the day. A bed partner is often the first person to notice the pattern. That is one reason sleep apnea can go undiagnosed for a long time.
3. What is the difference between sleep apnea and a sleep disorder?
Sleep apnea is one type of sleep disorder. The term sleep disorder is broader and includes many conditions that affect breathing, sleep timing, behavior, movement, or the ability to fall asleep and stay asleep. Sleep apnea specifically involves repeated breathing disruption during sleep. Other sleep disorders include insomnia, restless legs syndrome, parasomnias, and circadian rhythm disorders.
4. Is snoring always a sign of sleep apnea?
No. Snoring does not always mean someone has sleep apnea. Some people snore without having repeated breathing pauses. Still, loud or chronic snoring should not be brushed off automatically, especially if it is paired with gasping, dry mouth, morning headaches, or daytime fatigue. Snoring is a clue that may point to sleep-disordered breathing, but testing is needed for diagnosis.
5. What causes sleep apnea?
Obstructive sleep apnea usually happens when the upper airway narrows or collapses during sleep. This can be influenced by anatomy, body position, muscle tone, nasal obstruction, excess weight, alcohol use near bedtime, and other factors. Central sleep apnea is different because it involves unstable breathing signals from the brain rather than airway collapse.
6. What are the most common sleep disorders besides sleep apnea?
The most common sleep disorders besides sleep apnea include insomnia, restless legs syndrome, circadian rhythm sleep disorders, parasomnias, and hypersomnolence disorders such as narcolepsy. Each affects sleep in a different way. Some interfere with the ability to sleep, some disrupt timing, and others cause movement, unusual nighttime behavior, or excessive daytime sleepiness.
7. How is sleep apnea diagnosed?
Sleep apnea is diagnosed through clinical history and objective sleep testing. A clinician reviews symptom patterns, risk factors, and observations from the patient or a bed partner. If sleep apnea is suspected, testing usually involves a home sleep apnea test or an in-lab sleep study. The diagnosis is based on breathing-related findings during sleep, not symptoms alone.
8. What does a home sleep apnea test show?
A home sleep apnea test looks for breathing-related abnormalities during sleep. It usually measures airflow, breathing effort, oxygen levels, and pulse-related data. These tests can be useful when obstructive sleep apnea is suspected. However, they are more limited than a full lab sleep study and may not capture the full picture in more complex cases.
9. What is the difference between a home sleep test and a lab sleep study?
A home sleep test mainly focuses on breathing-related events and is often more convenient. A lab sleep study provides a more complete assessment by measuring brain waves, sleep stages, airflow, oxygen levels, muscle activity, heart rhythm, and often limb movements. Lab testing is more useful when the diagnosis is uncertain or when other sleep disorders may be involved.
10. What does AHI mean in sleep apnea?
AHI stands for apnea-hypopnea index. It describes how many breathing events occur per hour of sleep or recording time, depending on the test. It is commonly used to estimate sleep apnea severity. Still, AHI does not tell the whole story. Symptoms, oxygen changes, sleep fragmentation, body position, and REM-related patterns all matter too.
11. Can sleep apnea cause morning headaches?
Yes. Sleep apnea can contribute to morning headaches in some people. Repeated breathing disruption, fragmented sleep, oxygen fluctuations, and overnight stress-response activation may all play a role. Morning headaches are not specific to sleep apnea, but when they appear alongside snoring, dry mouth, or fatigue, sleep-disordered breathing should be considered.
12. Can sleep apnea cause brain fog and poor concentration?
Yes. Sleep apnea can affect attention, focus, memory, mental clarity, and daytime performance. Even when a person technically spends enough hours in bed, repeated breathing events and brief arousals can prevent sleep from feeling restorative. Many people describe this not as sleepiness, but as feeling flat, foggy, or not fully switched on.
13. What treatments are available for sleep apnea?
Sleep apnea treatment may include CPAP therapy, oral appliance therapy, positional therapy, weight management, lifestyle changes, and in some cases surgery. The right treatment depends on the severity and type of sleep apnea, the patient’s anatomy, symptoms, and ability to use the treatment consistently over time.
14. What is the best treatment for sleep apnea?
There is no one best treatment for everyone. CPAP is often highly effective, but some patients do better with oral appliance therapy, positional therapy, or a combination approach. The best treatment is the one that fits the clinical picture and can be used reliably with appropriate follow-up.
15. When should someone seek help for poor sleep?
Someone should seek help when poor sleep becomes persistent, affects daytime function, or comes with warning signs such as loud snoring, gasping, witnessed pauses in breathing, dry mouth, morning headaches, excessive daytime sleepiness, repeated insomnia, or unusual nighttime behavior. If sleep is affecting health, performance, or safety, it deserves evaluation.
Conclusion
Sleep disorders are easy to underestimate because they often show up as symptoms that seem unrelated to sleep. A person may focus on the headache, the brain fog, the snoring, the jaw tension, or the constant fatigue without realizing that the real story starts during the night.
That is what makes sleep apnea and other sleep disorders so important to understand. They can quietly disrupt breathing, recovery, cognition, mood, pain regulation, and overall health long before someone puts the pieces together. The encouraging part is that these conditions are not invisible once you know what to look for. The patterns can be recognized. The right testing can clarify what is happening. And treatment can make a real difference.
If your sleep leaves you feeling unrefreshed, mentally dull, physically tense, or concerned about what may be happening overnight, it is worth looking deeper. Better sleep is not just about getting more hours. It is about getting sleep that actually restores you.
Randy Clare is a writer, educator, and health communicator focused on making complex clinical topics easier to understand. Through The Sleep and Respiratory Scholar, he creates clear, practical content on bruxism, headache, sleep, airway health, and respiratory symptoms. He is the author of The Brux Method, President of ClenchAlert.com and host of The Clenching Chronicle Podcast, where he explores jaw tension, clenching, headaches, and behavior-based approaches to relief. His work helps readers better understand symptoms, recognize patterns, and take more informed next steps.





