Before delving deeper into the effects of bruxism and potential solutions, it’s essential to understand what bruxism is and the different forms it can take. Bruxism refers to the involuntary and often unconscious habit of grinding, gnashing, or clenching your teeth.
This condition affects a significant portion of the population, with studies estimating that 8-31% of adults and 14-20% of children experience bruxism at some point in their lives. It is important to note that the prevalence of bruxism tends to decrease with age.
There are two primary types of bruxism: awake bruxism and sleep bruxism. As the names suggest, these conditions differ based on when they occur.
Awake bruxism, also known as diurnal bruxism, typically involves teeth clenching or grinding during the day, often as a response to stress, anxiety, or even concentration. Individuals with awake bruxism may be unaware of their habit, as it often occurs subconsciously.
On the other hand, sleep bruxism, or nocturnal bruxism, occurs during sleep and is considered a sleep-related movement disorder. People who suffer from sleep bruxism may be entirely unaware of their teeth clenching and grinding until a partner or family member points it out, or they begin experiencing symptoms such as jaw pain, tooth damage, or headaches.
Sleep bruxism has been linked to other sleep disorders too, such as periodic limb movements and sleep apnea, they can significantly disrupt the quality of sleep.
While both types of bruxism can lead to similar consequences, the underlying causes and treatment approaches may differ.
Understanding the type of bruxism you’re experiencing is crucial for developing an effective treatment plan and finding relief from the associated symptoms.
Causes of Bruxism
Bruxism is a multifactorial condition with various contributing factors that can influence its onset and severity. Understanding these factors can help you and your healthcare provider develop a targeted treatment plan to alleviate the associated facial pain and headaches.
A. Psychological Factors
Stress and Anxiety: Stress and anxiety are significant contributors to bruxism, particularly in cases of awake bruxism. When you’re feeling overwhelmed or anxious, you might subconsciously clench your teeth or grind them together as a coping mechanism. Prolonged periods of stress can exacerbate this habit, leading to worsening symptoms.
Emotions and Personality Traits: Certain emotions and personality traits, such as anger, frustration, or competitiveness, can also contribute to teeth clenching and grinding. Individuals with these traits may be more prone to bruxism due to their heightened emotional states or difficulty managing stress.
B. Physical Factors
Sleep Disorders: Sleep bruxism is often associated with sleep disorders, such as sleep apnea or periodic limb movement disorder. These conditions can disrupt normal sleep patterns, leading to involuntary muscle movements, including teeth grinding and nighttime clenching.
Abnormal Bite and Dental Issues: An abnormal bite or misaligned teeth can cause uneven pressure distribution when the jaw is closed, potentially leading to bruxism. In some cases, dental issues such as missing or crooked teeth can contribute to teeth grinding and clenching.
Genetics and Heredity: Bruxism can run in families, with research suggesting a genetic component to the condition. If a close family member has bruxism, you may be at a higher risk of developing the condition yourself.
C. Lifestyle Factors
Alcohol and Caffeine Consumption: Excessive alcohol and caffeine consumption can increase the likelihood of bruxism. Alcohol can disrupt sleep patterns, while caffeine acts as a stimulant, making it more challenging to relax the jaw muscles.
Tobacco Use: Smoking has been linked to an increased risk of bruxism, particularly sleep bruxism. The stimulating effects of nicotine, combined with its impact on sleep quality, can contribute to teeth grinding and clenching.
Certain Medications: Some medications, including specific antidepressants and antipsychotics, can have side effects that increase the risk of bruxism. If you suspect your medication is contributing to your teeth grinding or clenching, it’s essential to discuss this with your healthcare provider. They may recommend adjusting your dosage or exploring alternative treatment options.
By considering the various factors that contribute to bruxism, you can work with your healthcare provider to identify the most likely causes and develop a personalized treatment plan to address your symptoms effectively.
Symptoms and Diagnosis
Recognizing the symptoms of bruxism and seeking an accurate diagnosis are crucial first steps in finding relief from the associated facial pain and headaches. Here’s what to look for to diagnose bruxism and what to expect during the diagnosis process:
A. Common Symptoms
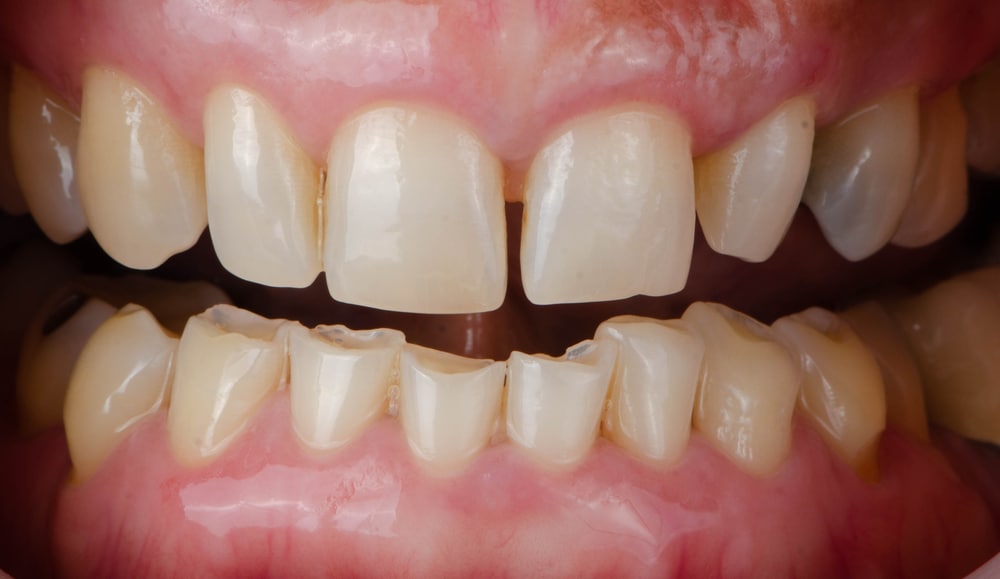
Tooth Wear and Damage: One of the most evident signs of bruxism is the wear and tear on your teeth. Constant grinding and clenching can cause your teeth to become worn down, chipped, or fractured, leading to increased sensitivity and a higher risk of dental complications.
Facial Pain and Temporomandibular Joint (TMJ) Issues: Bruxism can put a tremendous strain on the jaw muscles and the TMJ, resulting in pain, stiffness, and difficulty opening or closing your mouth. This discomfort can also radiate to the face and neck.
Headaches and Earaches: The strain on the jaw muscles caused by bruxism can lead to tension headaches, which are often felt around the temples, forehead, and back of the head. Additionally, bruxism can cause earaches due to the proximity of the TMJ to the ear canal.
Sleep Disruptions: Sleep bruxism can disrupt your sleep and that of your partner, leading to poor sleep quality, daytime fatigue, and irritability.
B. Diagnosis Process
Dental Examination: If you suspect you have bruxism, the first step is to consult with your dentist. They will perform a thorough examination of your teeth, jaw, and bite to assess for signs of wear, damage, or misalignment.
Patient History and Symptom Evaluation: Your dentist will also review your medical and dental history, as well as discuss any symptoms you’re experiencing. This information will help them determine if bruxism is the cause of your discomfort and identify any potential contributing factors.
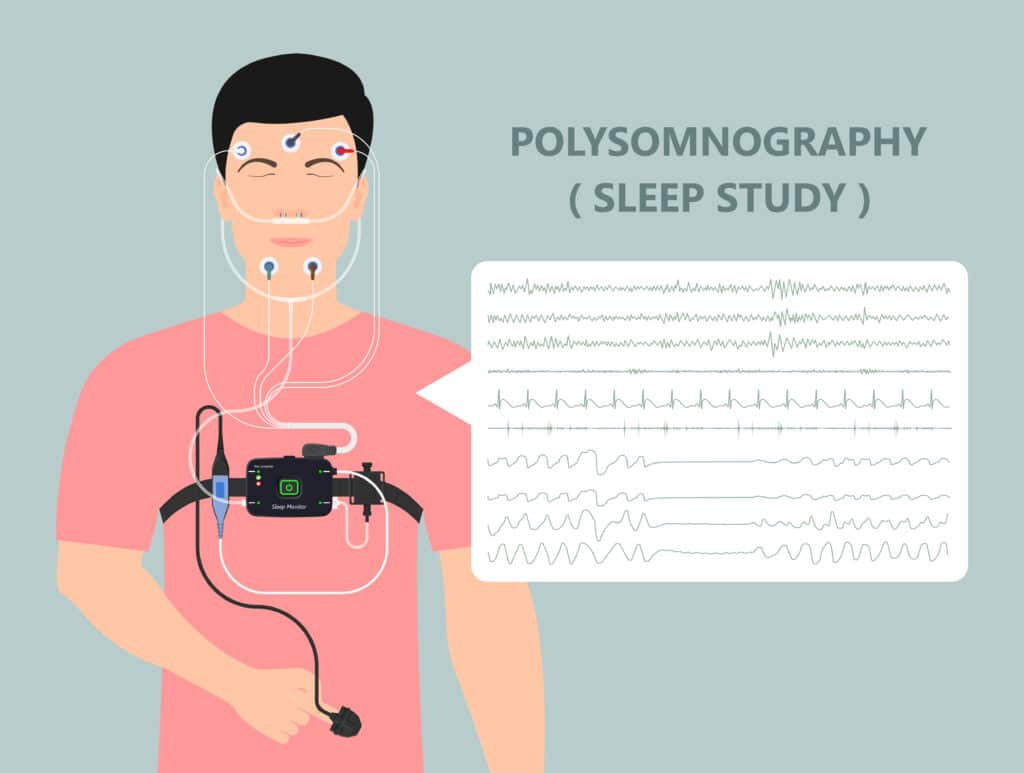
Sleep Study (Polysomnography) for Sleep Bruxism: If your dentist suspects sleep bruxism, they may recommend a sleep study, or polysomnography, to diagnose bruxism. This test records various physiological data while you sleep, such as brain activity, eye movement, heart rate, and muscle activity, providing insight into the presence and severity of sleep bruxism.
By identifying the symptoms of bruxism and obtaining a thorough diagnosis, you can begin the journey toward relief from jaw pain, headaches, and other related discomforts.
Complications of Bruxism
Left untreated, bruxism can lead to various complications that can significantly impact your oral health, sleep, and overall quality of life. It’s essential to be aware of these potential complications and seek treatment to prevent or manage them effectively.
A. Dental Complications
Tooth Fractures and Loss: The constant grinding and clenching of teeth can cause excessive wear, fractures, and even tooth loss. These dental issues can be painful, affect your ability to chew and speak, and require extensive dental treatment, such as crowns, root canals, or implants.
Tooth Sensitivity: As your teeth wear down due to bruxism, the protective enamel layer becomes thinner, exposing the more sensitive inner layers of the tooth. This exposure can result in increased tooth sensitivity, making it uncomfortable to consume hot, cold, or sweet foods and beverages.
B. Temporomandibular Joint (TMJ) Disorders
The repetitive strain on the jaw muscles and TMJ caused by bruxism can lead to the development of TMJ disorders. These conditions can cause pain, stiffness, and limited mobility in the jaw, as well as clicking or grinding noises or popping sounds when opening or closing your mouth. In severe cases, these disorders can be debilitating and require extensive treatment, such as physical therapy, medication, or surgery.
C. Sleep Disturbances
Sleep bruxism can disrupt your sleep and that of your partner, leading to poor sleep quality and increased daytime fatigue. Over time, these sleep disturbances can contribute to a range of health issues, such as mood disorders, weakened immune function, and an increased risk of chronic conditions like cardiovascular disease and diabetes.
D. Impact on Quality of Life
The various complications associated with bruxism can significantly impact your quality of life. Persistent jaw pain, headaches, and dental issues can make daily activities like eating, talking, and sleeping uncomfortable and challenging. Moreover, the ongoing stress and discomfort of sleep related bruxism can affect your mental and emotional well-being, leading to feelings of frustration, anxiety, and depression.
By addressing bruxism and its associated complications, you can improve your oral health, sleep quality, and overall well-being. Seeking appropriate treatment and implementing preventive measures can help alleviate the symptoms of bruxism, reducing the risk of long-term complications and enhancing your quality of life.
Treatment Options
Effectively managing bruxism and its associated symptoms requires a comprehensive and personalized treatment approach. Depending on the severity and underlying causes of your condition, your healthcare provider may recommend a combination of dental interventions, behavioral therapies, medications, and lifestyle modifications.
A. Dental Interventions
Night guards, mandibular advancement devices and occlusal splints: One of the most common treatments for bruxism is the nightly use of a night guard or occlusal splint. These custom-fitted dental appliances are worn during sleep to provide a protective barrier between the upper and lower teeth, preventing damage and reducing the strain on the jaw muscles and TMJ.
Mandibular advancement devices consist of an upper and lower night guard that are connected and adjustable to position the jaw during sleep to reduce or eliminate sleep apnea. This is an excellent treatment for mild to moderate obstructive sleep apnea that will also treat sleep bruxism that is related to untreated obstructive sleep apnea.
Dental Correction: In cases where an abnormal bite or dental issues contribute to bruxism, your dentist may recommend orthodontic treatment, such as braces or clear aligners, to correct your bite and alleviate teeth grinding and clenching.

B. Behavioral and Relaxation Therapies
Cognitive-Behavioral Therapy (CBT): CBT is a type of psychotherapy that can help you identify and change negative thought patterns and behaviors contributing to bruxism, such as stress and anxiety.
Biofeedback: Biofeedback is a technique that teaches you to control your body’s physiological responses, such as muscle tension, by providing real-time feedback on these functions. This approach can help you learn to relax your jaw muscles and reduce teeth grinding and clenching.
Stress Management and Relaxation Techniques: Practicing stress management and relaxation techniques, such as deep breathing, meditation, or yoga, can help you manage stress and anxiety, which may contribute to bruxism.
C. Medications
Muscle Relaxants: Your healthcare provider may prescribe muscle relaxants to be taken before bedtime to help relax the jaw muscles and reduce teeth grinding during sleep.
Anti-Anxiety Medications: In some cases, anti-anxiety medications, such as selective serotonin reuptake inhibitors (SSRIs), may be prescribed to address anxiety-related bruxism.
Botox Injections: Botox injections can be used to weaken the jaw muscles temporarily, reducing the force of teeth grinding and clenching. This treatment may provide relief for those with severe bruxism that hasn’t responded to other therapies.
D. Lifestyle Modifications
Reducing Caffeine and Alcohol Intake: Cutting back on caffeine and alcohol consumption can help reduce the risk of bruxism by promoting relaxation and improving sleep quality.
Smoking Cessation: Quitting smoking can help reduce the risk of sleep bruxism and improve overall health.
Establishing a Regular Sleep Schedule: Maintaining a consistent sleep schedule and creating a relaxing bedtime routine can promote better sleep quality and help reduce the occurrence of sleep bruxism.
By exploring a range of treatment options and working closely with your healthcare provider, you can develop a personalized plan to effectively manage bruxism and find relief from the associated facial pain and headaches.
Prevention Strategies
While treating bruxism is essential, implementing prevention strategies can help reduce the risk of developing the condition or prevent it from worsening. Incorporating stress reduction techniques, maintaining good dental care, and staying aware of your teeth grinding and clenching habits are all crucial components of a prevention plan.
A. Stress Reduction Techniques
Meditation and Mindfulness: Practicing meditation and mindfulness can help you manage stress and anxiety more effectively, reducing the likelihood of teeth grinding and clenching. By focusing on the present moment and learning to observe your thoughts and emotions without judgment, you can develop greater emotional resilience and better coping skills for awake bruxism.
Exercise and Physical Activity: Engaging in regular exercise and physical activity can provide a natural outlet for stress and promote the release of endorphins, which are chemicals in the brain that help improve mood and reduce feelings of anxiety. Establishing a consistent exercise routine can help keep stress levels in check and reduce the risk of bruxism.
B. Dental Care and Regular Check-ups
Maintaining good oral hygiene and visiting your dentist for regular check-ups can help prevent dental issues that may contribute to bruxism, such as tooth misalignment or an abnormal bite. Your dentist can also monitor for early signs of teeth grinding or clenching, allowing for prompt intervention to prevent further damage or complications.
C. Awareness of Teeth Grinding and Jaw Clenching Habits
Becoming aware of your teeth grinding habit, particularly for awake bruxism, can help you take proactive steps to break the cycle. Pay attention to situations where you’re more likely to grind your teeth or clench your jaw, such as when you’re stressed, concentrating, or engaged in other triggering activities.
Once you’re aware of these habits, you can consciously work to relax your jaw and practice healthier coping mechanisms, such as deep breathing or muscle relaxation techniques.
By focusing on prevention strategies, you can minimize the risk of developing bruxism or prevent it from worsening, ultimately protecting your oral health and overall well-being. Regularly practicing stress reduction techniques, maintaining good dental care, and staying mindful of your teeth grinding and clenching habits can go a long way in ensuring a healthier, dental pain–free future.
Home Remedies and Self-Care
In addition to professional treatment and prevention strategies to treat bruxism, incorporating home remedies and self-care practices into your daily routine can help alleviate jaw pain and headaches associated with bruxism. Here are some simple yet effective techniques to help manage your symptoms at home:
A. Jaw Exercises and Stretching
Performing gentle jaw exercises and stretches can help strengthen and relax your jaw muscles, reducing tension and discomfort. Consult with your dentist or a physical therapist for specific exercises tailored to your needs, and be sure to perform them consistently to see the best results.
B. Applying Ice or Heat Packs
Applying ice or heat packs to the affected area can help relieve pain and inflammation caused by bruxism. An ice pack can be particularly useful for acute pain, while a heat pack can help relax tense muscles and improve circulation. Remember to always wrap the pack in a cloth or towel before applying it to your skin to avoid burns or frostbite.
C. Massaging Jaw Muscles
Massaging your jaw muscles can help alleviate pain and tension associated with bruxism. Gently press your fingers on the sore areas of your jaw and use small, circular motions to massage the muscles. You can also use a warm towel or a massage tool designed specifically for the sore jaw muscles to enhance the effects of the massage.
D. Avoiding Hard and Chewy Foods
Consuming hard and chewy foods can exacerbate jaw pain and tension caused by bruxism. Opt for softer foods that require less jaw movement and force, such as cooked vegetables, smoothies, and soups. Avoid chewing gum as the constant movement can trigger jaw pain. As your symptoms improve, you can gradually reintroduce these foods into your diet.
E. Practicing Proper Jaw Alignment
Being mindful of your jaw alignment can help reduce the strain on your jaw muscles and TMJ. Maintain a relaxed jaw position by keeping your lips together and teeth slightly apart with your tongue resting on the roof of your mouth.
This neutral position can help minimize teeth grinding and clenching, ultimately reducing jaw pain and headaches.
By incorporating these home remedies and self-care practices into your daily routine, you can take an active role in managing your bruxism symptoms and find relief from jaw pain and headaches. Remember, always consult with your healthcare provider before starting any new self-care practices to ensure they are safe and appropriate for your specific needs.
Pediatric Bruxism
Bruxism is not exclusive to adults; children can also experience teeth grinding and clenching. It’s crucial to understand the unique characteristics of pediatric bruxism and how to address it effectively to ensure the long-term oral health and well-being of baby teeth and your child.
A. Prevalence and Characteristics in Children
Pediatric bruxism affects up to 30% of children, with the highest prevalence in those aged 3-6 years. Similar to adults, children can experience both awake and sleep bruxism episodes. However, unlike adult bruxism, most children outgrow their teeth grinding habits as they reach adolescence, often without any long-term consequences.
B. Causes and Potential Risk Factors
Stress and Anxiety in Children: Just like adults, children can experience stress and anxiety, which may manifest as bruxism. Common stressors for children include family issues, school-related concerns, and social pressures.
Sleep Disorders and Sleep-Related Breathing Issues: Sleep disorders, such as sleep apnea or restless leg syndrome, can increase the risk of sleep bruxism in children. Additionally, sleep-related breathing issues, like snoring or nasal congestion, can contribute to teeth grinding during sleep.
Developmental Factors: Pediatric bruxism can sometimes be a part of a child’s normal development as they grow and their teeth and jaws change. In many cases, this type of bruxism resolves on its own as the child matures.
C. Treatment and Management in Children
Parental Support and Stress Reduction: Parents can play a critical role in helping their child manage stress and anxiety. Providing a supportive and nurturing environment, encouraging open communication, and helping your child develop healthy coping strategies can all contribute to reducing bruxism.
Dental Interventions as Needed: Depending on the severity and impact of your child’s bruxism, dental interventions such as mouthguards or splints may be necessary. Consult with your child’s dentist to determine the most appropriate course of action.
Monitoring and Regular Dental Check-ups: Regular dental check-ups can help ensure that any signs of bruxism are detected early and addressed promptly. Your child’s dentist can monitor their oral health, provide guidance on managing bruxism, and recommend any necessary treatments.
By understanding the unique aspects of pediatric bruxism and working closely with your child’s healthcare provider, you can effectively manage and treat your child’s teeth grinding and clenching habits, ensuring they maintain good oral health throughout their development.
Prognosis and Long-term Effects
The prognosis for bruxism varies depending on the individual and the underlying causes of their teeth grinding and clenching habits. Understanding the potential for spontaneous improvement, the impact of chronic bruxism on oral health, and the importance of ongoing management and treatment is crucial for maintaining overall well-being.
A. Potential for Spontaneous Improvement
In some cases, bruxism may improve spontaneously without the need for medical intervention. This is particularly true for children, who often outgrow teeth grinding habits as they develop. For adults, bruxism may resolve on its own if the underlying cause, such as stress or a specific medication, is addressed. However, it’s important not to rely solely on spontaneous improvement, as ongoing monitoring and treatment may still be necessary to prevent long-term complications.
B. Chronic Bruxism and its Impact on Oral Health
If left untreated, chronic bruxism can have significant consequences for your oral health. Persistent teeth grinding and clenching can lead to tooth wear, fractures, tooth mobility and sensitivity, as well as temporomandibular joint disorders.
Additionally, chronic bruxism can cause or exacerbate sleep disturbances, impacting your overall quality of life. For these reasons, it’s essential to seek professional help and engage in ongoing management and treatment to minimize the long-term effects of bruxism.
C. Importance of Ongoing Management and Treatment
Effectively managing bruxism often requires a combination of dental interventions, behavioral therapies, medications, and lifestyle modifications. The key to a successful outcome is ongoing management and treatment, tailored to your specific needs and circumstances. Regular dental check-ups, monitoring of symptoms, and adjustments to your treatment plan as needed can help ensure that bruxism is kept under control and that its impact on your oral health and overall well-being is minimized.
While bruxism may improve spontaneously in some cases, it’s crucial not to overlook the potential long-term effects and the importance of ongoing management and treatment. By working closely with your healthcare provider and following a comprehensive treatment plan, you can effectively manage your bruxism and enjoy a healthier, pain-free future.
Emerging Research and Future Directions
As our understanding of bruxism evolves, researchers continue to explore new diagnostic tools, treatment options, and the underlying causes of teeth grinding and clenching. By staying informed about the latest advances in bruxism research, you can be better prepared to make informed decisions about your own oral health and bruxism management.
A. Advances in Diagnostic Tools and Methods
Emerging diagnostic tools and methods are being developed to improve the accuracy and efficiency of bruxism diagnosis. For example, advances in digital imaging and dental wear analysis can provide more detailed information about tooth damage caused by tooth grinding and clenching. Additionally, improvements in sleep study technology, such as portable home sleep testing devices, can make it easier for patients to undergo evaluations for nocturnal bruxism.
B. Novel Treatment Options and Therapies
Researchers are continually exploring new treatment options and therapies for bruxism. For example, alternative therapies, such as acupuncture and low-level laser therapy, have shown promise in reducing the symptoms of bruxism in some studies. Additionally, the development of new medications or the repurposing of existing drugs could offer novel approaches to managing bruxism, particularly for those who do not respond well to traditional treatments.
C. Understanding the Role of Genetics and Heredity in Bruxism
The role of genetics and heredity in bruxism is an area of ongoing research. Some studies have suggested that there may be a genetic component to bruxism, with certain genes potentially predisposing individuals to teeth grinding and clenching. As our understanding of the genetic factors underlying bruxism grows, this knowledge could inform the development of more targeted and personalized treatments for those affected by the condition.
D. Relationship Between Bruxism and Other Health Conditions
The relationship between bruxism and other health conditions is another area of active research. Studies have found links between bruxism and various sleep disorders, such as gastroesophageal reflux disease (GERD), obstructive sleep apnea, and even certain neurological conditions and sleep related movement disorder. Further investigation into these connections could help healthcare providers develop more comprehensive treatment plans that address the broader context of a patient’s overall health, ultimately leading to improved outcomes for those with bruxism.
By staying informed about the latest research and emerging trends in bruxism diagnosis and treatment, you can make well-informed decisions about your own oral health and bruxism management. As the scientific community continues to deepen its understanding of this complex condition, new diagnostic tools, treatment options, and insights into the underlying causes of bruxism will undoubtedly contribute to more effective and personalized care for those affected by teeth grinding and clenching.
Conclusion
As we’ve explored throughout this article, bruxism is a complex and multifaceted condition that can have a significant impact on an individual’s oral health, overall well-being, and quality of life. In conclusion, it’s essential to emphasize the importance of early detection and intervention, the multifactorial nature of bruxism, the need for personalized treatment plans, and the role of education and awareness in prevention and management.
A. Importance of Early Detection and Intervention
Early detection and intervention are crucial for effectively managing bruxism and minimizing its long-term effects. By seeking professional help at the first signs of teeth grinding or clenching, you can help prevent complications such as tooth wear, TMJ disorders, and sleep disturbances. Regular dental check-ups and ongoing monitoring of your symptoms are key components of early detection and intervention.
B. The Multifactorial Nature of Bruxism
Bruxism is a multifactorial condition with a range of potential causes, including psychological factors, physical factors, and lifestyle factors. Understanding the unique combination of factors contributing to your bruxism is essential for developing a comprehensive and effective treatment plan tailored to your specific needs and circumstances.
C. Need for Personalized Treatment Plans
Given the multifactorial nature of bruxism, personalized treatment plans that address the underlying causes and individual circumstances are crucial for successful management. Such plans may involve a combination of dental interventions, behavioral therapies, medications, and lifestyle modifications. By working closely with your healthcare provider, you can create a customized treatment plan that best meets your needs and helps you find relief from bruxism-related jaw pain and headaches.
D. The Role of Education and Awareness in Prevention and Management
Education and awareness play a vital role in the prevention and management of bruxism. By understanding the causes, symptoms, and potential complications of bruxism teeth grinding and clenching, you can take proactive steps to address your bruxism and maintain good oral health. Additionally, raising awareness about bruxism among friends, family members, and healthcare providers can help others recognize the signs of this condition and seek appropriate care.
In conclusion, bruxism is a complex condition that requires early detection, a comprehensive understanding of its multifactorial nature, personalized treatment plans, and ongoing education and awareness for effective prevention and management. By staying informed and taking a proactive approach to your oral health, you can successfully manage your bruxism and enjoy a healthier, pain-free future.
References
Lobbezoo, F., Ahlberg, J., Glaros, A. G., Kato, T., Koyano, K., Lavigne, G. J., … & Winocur, E. (2013). Bruxism defined and graded: an international consensus. Journal of Oral Rehabilitation, 40(1), 2-4. https://doi.org/10.1111/joor.12011
Manfredini, D., Winocur, E., Guarda-Nardini, L., Paesani, D., & Lobbezoo, F. (2013). Epidemiology of bruxism in adults: a systematic review of the literature. Journal of Orofacial Pain, 27(2), 99-110. https://doi.org/10.11607/jop.921
Lavigne, G. J., Khoury, S., Abe, S., Yamaguchi, T., & Raphael, K. (2008). Bruxism physiology and pathology: an overview for clinicians. Journal of Oral Rehabilitation, 35(7), 476-494. https://doi.org/10.1111/j.1365-2842.2008.01881.x
Klasser, G. D., & Rei, N. (2010). Sleep bruxism: an overview for clinicians. Journal of Prosthodontics, 19(6), 453-461. https://doi.org/10.1111/j.1532-849X.2010.00614.x
Sateia, M. J. (2014). International classification of sleep disorders. Chest, 146(5), 1387-1394. https://doi.org/10.1378/chest.14-0970
Shetty, S., Pitti, V., Satish Babu, C. L., Surendra Kumar, G. P., & Deepthi, B. C. (2010). Bruxism: a literature review. Journal of Indian Prosthodontic Society, 10(3), 141-148. https://doi.org/10.1007/s13191-011-0061-3
Manfredini, D., & Lobbezoo, F. (2010). Relationship between bruxism and temporomandibular disorders: a systematic review of literature from 1998 to 2008. Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology, and Endodontology, 109(6), e26-e50. https://doi.org/10.1016/j.tripleo.2010.02.013
Macedo, C. R., Silva, A. B., Machado, M. A., Saconato, H., & Prado, G. F. (2007). Occlusal splints for treating sleep bruxism (tooth grinding). Cochrane Database of Systematic Reviews, (4). https://doi.org/10.1002/14651858.CD005514.pub2
Gungormus, Z., & Erciyas, K. (2009). Evaluation of the relationship between anxiety and depression and bruxism. Journal of International Medical Research, 37(2),
Lobbezoo, F., & Naeije, M. (2001). Bruxism is mainly regulated centrally, not peripherally. Journal of Oral Rehabilitation, 28(12), 1085-1091. https://doi.org/10.1046/j.1365-2842.2001.00839.x
Wetselaar, P., Vermaire, E. J. H., Lobbezoo, F., Schuller, A. A. (2019). The prevalence of awake bruxism and sleep bruxism in the Dutch adult population. Journal of Oral Rehabilitation, 46(7), 617-623. https://doi.org/10.1111/joor.12794
Carra, M. C., Huynh, N., & Lavigne, G. (2012). Sleep bruxism: a comprehensive overview for the dental clinician interested in sleep medicine. Dental Clinics of North America, 56(2), 387-413. https://doi.org/10.1016/j.cden.2012.01.006
Winocur, E., Gavish, A., Voikovitch, M., Emodi-Perlman, A., & Eli, I. (2006). Drugs and bruxism: a critical review. Journal of Orofacial Pain, 20(1), 75-84. https://pubmed.ncbi.nlm.nih.gov/16526916/
Van der Zaag, J., Lobbezoo, F., Wicks, D. J., Visscher, C. M., Hamburger, H. L., & Naeije, M. (2005). Controlled assessment of the efficacy of occlusal stabilization splints on sleep bruxism. Journal of Orofacial Pain, 19(2), 151-158. https://pubmed.ncbi.nlm.nih.gov/15895839/
Raphael, K. G., Sirois, D. A., Janal, M. N., Wigren, P. E., Dubrovsky, B., Nemelivsky, L. V., … & Lavigne, G. J. (2015). Sleep bruxism and myofascial temporomandibular disorders: a laboratory-based polysomnographic investigation. Journal of the American Dental Association, 146(11), 806-814. https://doi.org/10.1016/j.adaj.2015.02.014





