Experts estimate that nearly half of the adult population experiences headache disorders and 12% of Americans get migraine headaches.
Women are about three times more likely than men to experience migraine headaches.
There are several possible triggers for migraines, including stress, hormonal changes, certain foods or drinks, and environmental factors like noise and bright or flashing lights.
Migraine symptoms can include throbbing headache pain on one side of the head; nausea; vomiting; sensitivity to light and sound; blurred vision; difficulty concentrating; fatigue and dizziness.
The good news is that there are treatments available for migraine sufferers, such as medications to help prevent attacks from occurring or those designed to stop them when they do happen. Non-medication treatments may also be used, such as lifestyle changes (like exercising regularly), relaxation techniques (such as yoga or meditation) and cognitive behavior therapy
What is Migraine?
There are three main types of migraine headaches: migraine with aura, migraine without aura and chronic migraine.
migraines with aura occur when a sufferer experiences warning signs before an attack, such as flashes of light or blind spots. migraines without aura involve just the classic pain and related symptoms and can occur more frequently than migraines with aura.
Finally, chronic migraine is characterized by 15 or more migraine days per month, for at least three months in a row.
The four stages of a migraine include prodrome, aura, headache and postdrome.
Prodrome symptoms
Prodrome involves subtle changes that may warn you that a migraine is coming, such as mood changes or increased thirst.
Aura
Aura usually occurs after the prodrome and involves sensory disturbances, such as seeing flashes of light or having blind spots.
Headache
Headache is the third stage and is characterized by throbbing pain on one side of the head that can worsen with movement.
Postdrome
Postdrome occurs after an attack has ended and may involve feelings of confusion or exhaustion.
Migraines can be debilitating and interfere with your daily life. Knowing the different types, stages and triggers of migraines can help you to better manage your condition.
There are treatments available to both prevent and relieve migraine pain from occurring and stop them when they do happen.
If you think you may be suffering from migraine attacks, it’s important to speak to your doctor for a proper diagnosis and treatment plan.
Migraine Causes
Migraine headaches can be triggered by a variety of factors. Common migraine triggers include:
- Emotional stress is one of the most frequent causes of migraine headaches. During stressful situations, our brain releases certain compounds to fight against potential danger (known as the “flight or fight” response). The release of these chemicals can prompt a migraine. Other emotions such as anxiety, worry and excitement can intensify muscle tension and dilate blood vessels – both making migraines even more intense.
- Missing a meal. Skipping a meal or waiting too long to eat could be the catalyst for a migraine headache.
- Sensitivity to specific chemicals and preservatives in foods. Did you know that up to 30% of migraines may be triggered by certain foods and beverages? This includes aged cheese, alcoholic drinks, chocolate and food additives such as nitrates found in pepperoni, hot dogs and luncheon meats. Even fermented or pickled foods can act as triggers for migraine headaches.
- Caffeine. We can all be familiar with the throbbing ache of a caffeine-induced headache. When you deprive yourself of your daily dose, it seems that your body’s blood vessels become sensitive to it, triggering an unpleasant head pain when you go without it. Although some healthcare providers may recommend using caffeine as therapy for migraine treatment, this should not be done regularly or in large quantities.
- Daily use of pain-relieving medications. If you excessively rely on headache medications, that could lead to a “rebound” headache as your body becomes accustomed to the medication.
- Hormonal changes in women. Estrogen levels can be the cause of migraines in women, as they are more likely to occur around menstrual cycles and during times of hormonal shifts such as puberty or menopause. Birth control pills and hormone replacement therapy may also affect headaches. Young girls and post-menopausal women tend to experience fewer migraines due to the lack of estrogen fluctuation, however this does not apply to males suffering from migraine headaches. Following menopause, those stricken with hormonal-induced migraines may see a decrease over time in their headache frequency.
- Light. Whether you’re affected by flashing lights, fluorescent bulbs, the glow of your television or computer monitor, and even natural sunlight – all can be triggers for sensitivity.
- Migraine Triggers may also vary. Storm fronts, shifts in barometric pressure or altitude, wind gusts, and fatigue due to overwork or lack of restorative sleep can all be sources of discomfort and pain. Additionally, dieting without proper hydration intake as well as exposure to strong smells such as smoke and perfumes may trigger a migraine attack. Certain medications have been known to cause blood vessels to swell which is another possible factor that affects the onset of headaches.
The probability of experiencing a migraine headache is unpredictable, however, certain risk factors heighten the potentiality. For instance, those with a family history of migraines have an 80% chance of inheriting this condition; women between 15-55 years old tend to get more susceptible due to their hormones; stress plays an immense part in triggering off such headaches and smoking merely aggravates it further.
When it comes to warning signs of a migraine, the most common symptom is usually pain on one side of your head, which may throb or pulsate.
If you experience any of these signs, it’s important to take steps to prevent a Migraine attack from occurring. This can include avoiding known migraine triggers, getting enough sleep and relaxation, eating regularly, and keeping stress levels low.
Symptoms of a migraine
The most common symptom of a migraine headache is usually pain on one side of your head, which may throb or pulsate.
Other symptoms include nausea and vomiting; sensitivity to light and sound; blurred vision; difficulty concentrating; fatigue and dizziness.
Additionally, some people experience “prodrome” – subtle changes before an attack, such as mood changes or increased thirst. Migraines can also cause other neurological symptoms like numbness or tingling in your face or hands, hallucinations or disturbances of speech.
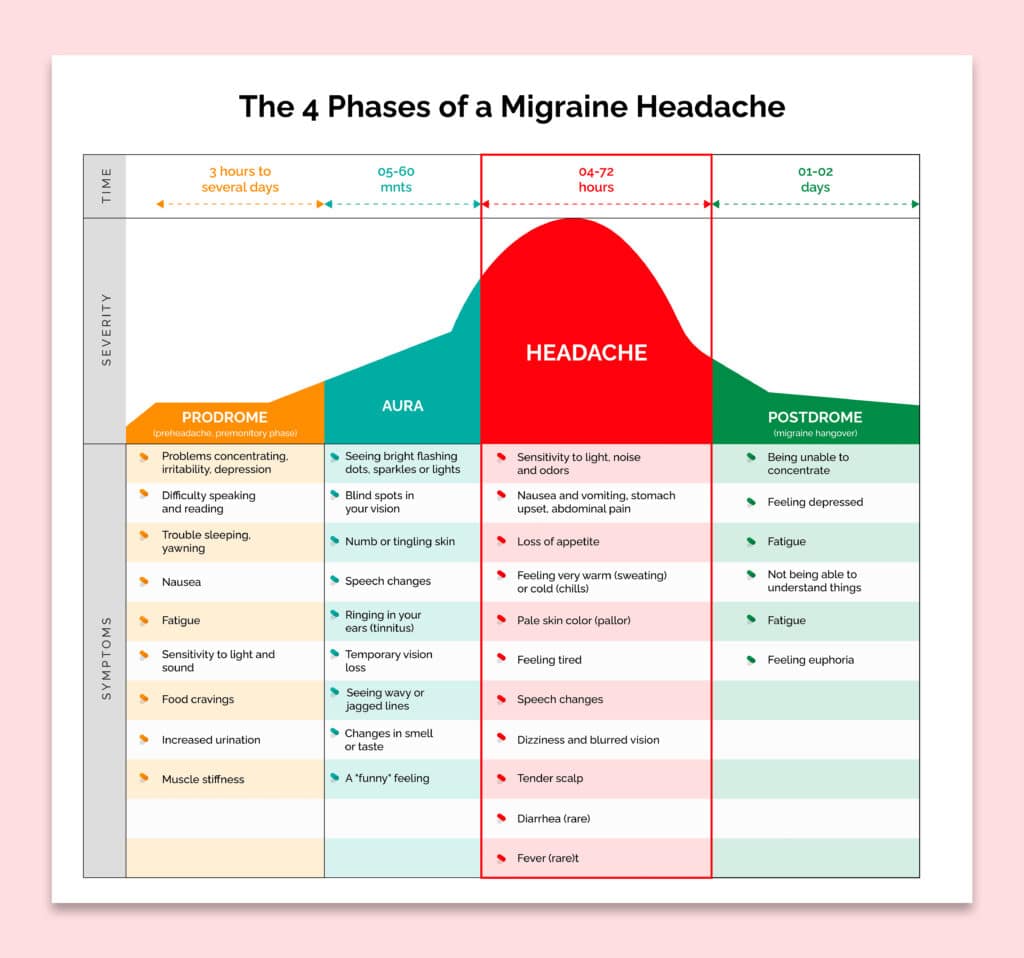
Prodrome
A few days before a migraine, you may experience slight alterations that indicate it is on the horizon. These clues could include constipation, fluctuations in your moods ranging from depression to elation, food cravings, tautness in the neck region, urination more than usual, bloating or water retention, and yawning frequently.
Aura
Have you ever experienced a migraine aura? Auras are temporary symptoms of the nervous system, and they can be both visual or other disturbances. Generally, they arise gradually and peak over several minutes up to an hour before fading away. Examples of possible auric manifestations include seeing shapes, bright spots, or flashes; partial blindness; tingling in the arm/legs; numbness on one side of your face; speaking difficulties – all signs that this is not your ordinary headache!
Migraine Attacks
From 4 to 72 hours, migraines may last without treatment. The frequency of migraine attacks varies per individual – they could occur rarely or even multiple times in one month. When a migraine strikes, you might experience pain on one or both sides of your head that pulses and throbs; plus sensitivity to different sensations such as sound, light, smell and touch; accompanied by nausea or vomiting.
Post-drome
After a migraine attack, you might feel drained, confused and washed out for up to a day. Some people report feeling elated. The sudden head movement might bring on the pain again briefly.
If you experience any of these Migraine symptoms or think that you may be suffering from Migraine, it’s important to speak to your doctor for a proper diagnosis and treatment plan.
Migraine frequency
The frequency of migraine could be once a year, once a week or any amount of time in between. Having two to four migraine headaches per month is the most common.
This is why the European Headache Federation described migraine as a “forgotten epidemic”.
Migraine is considered to be the first cause of disability in people under 50. And ranks second behind lower back pain as the leading cause of disability in the Global Burden of Disease (2016) study.
Treating migraines
If you suffer from mild to moderate migraines, then over-the-counter pain medication may be a dependable strategy.
Common components such as ibuprofen, aspirin, acetaminophen, naproxen and caffeine are found in these remedies.
If the FDA’s approval is essential for your situation, look no further than Excedrin® Migraine , Advil® Migraine and Motrin® Migraine Pain – all proven solutions recommended by medical experts worldwide to treat migraines.
Exercise caution when utilizing over-the-counter pain medications. Prolonged use may cause rebound headaches, or even lead to dependency issues.
If you find that the need is arising more than two to three times a week, tell your healthcare provider immediately.
They could recommend custom prescription medication which might be more successful in managing chronic pain and discomfort due to severe migraines.
Prescription drugs for migraine headaches include:
Triptan class of drugs (these are abortives):
- Sumatriptan.
- Zolmitriptan.
- Naratriptan.
Calcium channel blockers:
- Verapamil.
Calcitonin gene-related (CGRP) monoclonal antibodies:
- Erenumab.
- Fremanezumab.
- Galcanezumab.
- Eptinezumab.
Beta blockers:
- Atenolol.
- Propranolol.
- Nadolol.
Antidepressants:
- Amitriptyline.
- Nortriptyline.
- Doxepin.
- Venlafaxine.
- Duloxetine.
Antiseizure drugs:
- Valproic acid.
- Topiramate.
Other:
- Steroids.
- Phenothiazines.
- Corticosteroids.
Your healthcare provider might recommend vitamins, minerals, or herbs, including:
- Riboflavin (vitamin B2).
- Magnesium.
- Feverfew.
- Butterbur.
- Co-enzyme Q10.
Treating your migraine pain is made easier with the number of formulations available, such as pills, tablets, injections, suppositories and nasal sprays.
After consulting with a healthcare provider to identify what will work best for you specifically – medication type and combination of medications – you can take advantage of these solutions suited to combatting your unique headache pain.
To combat nausea, physicians may also prescribe drugs for maximum relief.
All medicines should be taken as prescribed by a headache specialist or healthcare provider with expertise in migraine care.
As you would with any other medication, it is imperative to read the instructions on the label and comply with your health practitioner’s advice completely.
If you’re looking for ways to manage your condition, home remedies are a great place to start for preventive treatment.
Try resting in a peaceful and tranquil room with cool temperatures; applying either heat or cold compresses onto your neck or forehead; massaging your scalp; practicing yoga, meditating, and/or biofeedback activities such as deep breathing exercises to help stay calm and relaxed; even gently pressing on the temples using circular motions.
What’s biofeedback?
Through the use of sophisticated equipment which can be affixed to your head, Biofeedback helps you monitor and manage physical tension in your body.
Alerts will sound when it detects stress levels rising so that these physiological processes are modified before they become overwhelming.
Eventually, with practice and repetition, individuals (children included) no longer require the device as they have learned to identify signs of tension on their own accord.
When to see a doctor
Do you experience migraine-like headaches, frequent migraines or other migraine symptoms but have yet to find relief? Keeping track of your symptoms and noting any changes or unique experiences may help guide an appropriate diagnosis.
Make a doctor’s appointment soon after recognizing the signs, as migraines left untreated can be detrimental to your overall health. Furthermore, if at anytime the pain suddenly feels different or more intense than before, seek medical attention immediately!
Warning indicators include:
A thunderclap-like headache, aching accompanied by fever, stiffness in the neck, confusion, seizures or double vision might be indicative of a stroke.
If you experience any numbness or weakness in your body following a head injury along with an ache that worsens after coughing, straining or sudden movement – seek medical attention immediately.
Remember: if you are fifty years and above and develop new pain related to headaches – do not ignore it!
Conclusion
Migraine headaches can often be managed with medications and lifestyle modifications.
However, it is important to understand migraine risk factors and discuss your symptoms and treatment options with your healthcare provider to make sure you have the most effective plan for managing your migraine pain.
With an appropriate treatment plan, migraines can be relieved quickly and effectively so you can get back to living life headache free!
Migraines are a common condition that affects millions of people. While there is no cure for migraine headaches, they are manageable with the right combination of medication, lifestyle changes, and alternative therapies such as biofeedback or yoga. Speak to your healthcare provider about the best treatment plan for you and explore different strategies for relieving migraine pain. With an appropriate migraine management plan, you can live a life free of migraine headaches.